Pigmentation in Indian Skin: Causes, Myths, and Treatment Do’s & Don’ts
Table of Contents
- Why Pigmentation Is So Common in Indian Skin
- High Baseline Melanin Activity in Indian Skin
- Year-Round UV Exposure in India
- Heat and Humidity as Independent Pigmentation Triggers
- Pollution and Environmental Stress
- Hard Water and Skin Barrier Damage
- Common Types of Pigmentation Seen in Indian Skin
- Biggest Myths About Pigmentation in Indian Skin
- The Right Way to Treat Pigmentation in Indian Skin
- Daily Skincare Routine for Pigmentation-Prone Indian Skin
- When Professional Treatment Is Needed
- Science-Backed Insights on Pigmentation in Indian Skin
- Final Thoughts
- References
- FAQS
Pigmentation is one of the most common skin concerns among Indians, yet it is also one of the most misunderstood. Many people follow aggressive routines, rely on fairness creams, or jump between home remedies and clinic treatments—only to see pigmentation worsen over time.

This is not because Indian skin is “weak.”
It’s because Indian skin behaves differently.
If you’ve read our earlier article on Asian skin discoloration, you already understand that melanin activity, inflammation, heat, and visible light play a major role. This article goes a step further. It focuses specifically on Indian skin, where climate, lifestyle, cultural practices, and common skincare myths significantly influence pigmentation outcomes.
This guide explains why pigmentation is so persistent in Indian skin, what mistakes make it worse, and the safe, evidence-based do’s and don’ts that actually work.
Why Pigmentation Is So Common in Indian Skin
Pigmentation in Indian skin is not caused by a single factor. It is the result of multiple overlapping triggers that act continuously.
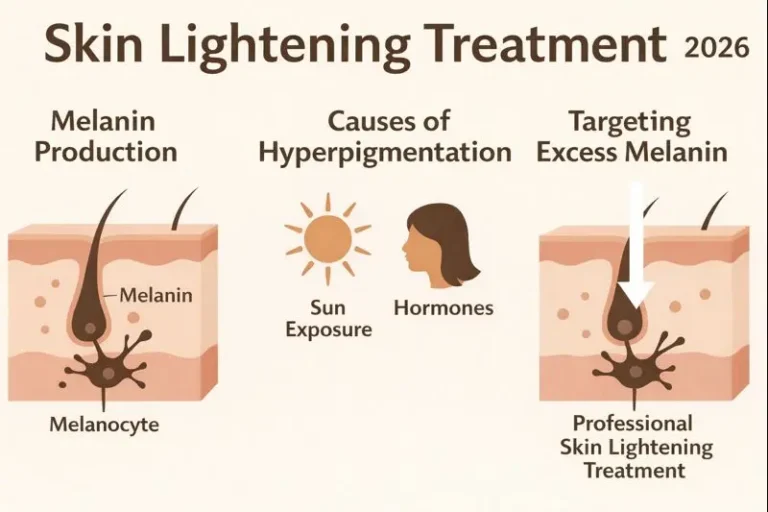
1. High Baseline Melanin Activity
Indian skin falls largely between Fitzpatrick skin types IV and V. This means melanocytes are naturally more active and respond strongly to any form of stimulation.
When Indian skin experiences:
- Acne
- Sun exposure
- Heat
- Friction
- Irritation
melanin production increases rapidly and remains elevated longer.
This explains why even small pimples leave long-lasting marks.
2. Year-Round UV Exposure
Unlike temperate climates, India has high UV index levels for most of the year.
Even on cloudy days, UV radiation remains strong. Daily exposure accumulates silently, darkening existing pigmentation and slowing healing.
Many people underestimate:
- UV exposure while commuting
- Exposure during early morning or evening
- Reflected UV from concrete and roads
This constant exposure is a major driver of pigmentation persistence.
3. Heat and Humidity as Independent Triggers
Heat plays a larger role in Indian skin than most people realize.
Cooking, outdoor temperatures, steam, and humidity increase:
- Blood flow to the skin
- Inflammatory signaling
- Melanocyte activation
This is why pigmentation often worsens in summer, even with sunscreen use.
Heat-induced pigmentation is especially relevant in Indian households where exposure is daily and unavoidable.
4. Pollution and Environmental Stress
Urban Indian environments expose skin to:
- Particulate matter
- Heavy metals
- Oxidative stress
These pollutants disrupt the skin barrier and trigger low-grade inflammation, which stimulates melanin production over time.

Pollution-related pigmentation is often dull, diffuse, and resistant to treatment unless barrier repair is addressed.
5. Hard Water and Barrier Damage
Many regions in India have hard water with high mineral content.
Hard water:
- Weakens the skin barrier
- Increases dryness and irritation
- Makes skin more reactive
This chronic barrier disruption creates the perfect environment for pigmentation to persist or worsen.
Common Types of Pigmentation Seen in Indian Skin
Pigmentation in Indian skin is rarely uniform. Multiple types often coexist.
Post-Inflammatory Hyperpigmentation (PIH)
PIH is extremely common after acne, insect bites, rashes, or cosmetic procedures.
In Indian skin:
- PIH appears darker
- Penetrates deeper
- Takes longer to fade
This is why acne marks often linger for months.
Learn from complete guide on Post-Inflammatory Hyperpigmentation: What Causes It and How to Treat It Faster.
Melasma
Melasma affects a large number of Indian women, particularly during:
- Pregnancy
- Hormonal changes
- Oral contraceptive use
Indian melasma tends to:
- Cover larger facial areas
- Worsen with heat
- Recur easily
Read detailed research by Dr. Faiza Shams on why melasma keeps coming back.
Sun-Induced and Heat-Induced Pigmentation
Repeated sun and heat exposure leads to gradual darkening of:
- Forehead
- Cheeks
- Perioral area
- Jawline
This pigmentation often looks uneven rather than spot-like.
Biggest Myths About Pigmentation in Indian Skin
This is where many treatment failures begin.

Myth 1: Fairness creams cure pigmentation
Most fairness creams:
- Do not address inflammation
- Do not protect against UV or heat
- Often contain irritants
They may temporarily brighten the skin surface but worsen pigmentation long term.
Myth 2: Natural remedies are always safe
Lemon, baking soda, toothpaste, and scrubs are commonly used at home.
These cause:
- Skin irritation
- Barrier damage
- Increased inflammation
Which leads to darker pigmentation, not lighter skin.
Myth 3: Scrubbing removes dark spots
Scrubbing creates micro-inflammation.
In Indian skin, this triggers melanocytes and worsens discoloration.
Pigmentation should never be treated with friction.
Myth 4: Strong treatments work faster
Aggressive peels, high-strength acids, and frequent lasers often cause:
- Rebound pigmentation
- PIH
- Melasma flares
Gentle, consistent treatment works better for Indian skin.
The Right Way to Treat Pigmentation in Indian Skin
The goal is not to “strip pigment.”
The goal is to calm the skin and regulate melanin production.

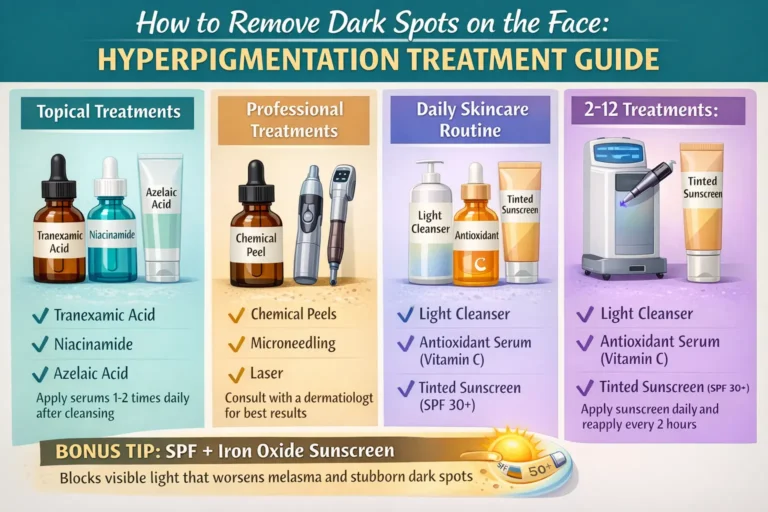
Treatment Do’s for Indian Skin
Do protect your skin daily
- Broad-spectrum SPF 30–50
- Reapply when outdoors
- Use hats and shade
Sunscreen is not optional.
Do focus on barrier repair
Healthy skin fades pigment faster.
Ingredients that help:
- Ceramides
- Glycerin
- Panthenol
- Niacinamide
Do use pigment-regulating ingredients
Safer options include:
- Azelaic acid
- Tranexamic acid
- Vitamin C (gentle formulations)
- Low-strength retinoids
Introduce actives slowly.
Do control heat exposure
Avoid:
- Hot showers
- Steam facials
- Excessive sun and heat
Heat management is essential for Indian skin.
Treatment Don’ts for Indian Skin
Don’t over-exfoliate
More exfoliation equals more inflammation.
Don’t mix too many actives
Layering acids, retinoids, and peels increases irritation.
Don’t self-prescribe strong treatments
Especially steroids, bleaching agents, or frequent peels.
Don’t expect overnight results
Pigmentation fades gradually. Speed often leads to relapse.
Daily Skincare Routine for Pigmentation-Prone Indian Skin
Morning
- Gentle cleanser
- Niacinamide or vitamin C
- Broad-spectrum sunscreen (tinted if melasma-prone)
Evening
- Gentle cleanser
- Azelaic acid or tranexamic acid
- Retinoid (2–3 nights weekly)
- Moisturizer
Consistency matters more than strength.
When Professional Treatment Is Needed
Consult a dermatologist if:
- Pigmentation worsens despite routine care
- Dark patches turn gray or blue
- You have recurrent melasma
- You develop PIH after procedures
Early guidance prevents long-term damage.
Science-Backed Insights on Pigmentation in Indian Skin
Recent dermatology research confirms:
- Indian skin melanocytes respond more strongly to inflammation
- Heat is a major independent trigger
- Barrier repair improves pigmentation outcomes
- Gentle treatment outperforms aggressive approaches
These findings explain why many conventional approaches fail.
Final Thoughts
Pigmentation in Indian skin is common, complex, and manageable. The key is understanding that Indian skin responds differently to heat, inflammation, and treatment intensity. Pigmentation fades best when the skin is protected, calm, and supported—not attacked.
When treated with patience and science-backed strategies, Indian skin can achieve long-term clarity without damage.
References
- Taylor S.C., et al. “Pigmentary Disorders in Skin of Color.” Dermatologic Clinics, 2022–2024.
- Grimes P.E., et al. “Post-Inflammatory Hyperpigmentation and Melasma in Brown Skin.” Journal of Clinical and Aesthetic Dermatology, 2021–2023.
- Passeron T., et al. “Heat, UV, and Pigmentation Pathways.” Journal of the European Academy of Dermatology, 2022–2024.
FAQS
1. Why is pigmentation more common in Indian skin?
Pigmentation is more common in Indian skin because melanocytes are naturally more active and respond strongly to inflammation, heat, and UV exposure. Factors like high sun intensity, humidity, pollution, and hormonal changes further increase pigmentation risk.
2. Does pigmentation in Indian skin fade on its own?
Some mild pigmentation may fade over time, but most pigmentation in Indian skin does not clear completely without treatment. Without sun protection and barrier-friendly skincare, dark spots often persist or return.
3. What is the safest treatment for pigmentation in Indian skin?
The safest treatment for pigmentation in Indian skin includes daily sunscreen, barrier repair, and gentle pigment-regulating ingredients like azelaic acid, niacinamide, tranexamic acid, and low-strength retinoids. Aggressive treatments often worsen pigmentation.
4. Why do home remedies worsen pigmentation in Indian skin?
Many home remedies like lemon, baking soda, or scrubs cause irritation and barrier damage. In Indian skin, this inflammation activates melanocytes and leads to darker, longer-lasting pigmentation instead of improvement.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810