Visible Light and Blue Light: The Hidden Triggers Making Pigmentation Worse Indoors
Table of Contents
Many people do everything “right.”
They wear sunscreen.
They avoid the sun.
They manage heat exposure.

Yet pigmentation still darkens. Visible light exposure is one of the most overlooked reasons why your pigmentation is not improving, even when you are using sunscreen daily. What skin pigmentation actually is can be understood as the natural coloring of the skin, caused by melanin production, which helps protect the skin from environmental and light-related damage.
This leads to a growing and confusing question in dermatology:
Why does pigmentation worsen indoors, even without sun or heat exposure?
The answer lies in visible light and blue light—a trigger that traditional skincare advice often overlooks.
Visible light, especially high-energy visible (HEV) blue light, can activate pigment pathways in the skin. This effect is particularly strong in melasma-prone individuals and deeper skin tones.
As Dr. Faiza Shams explains:
“Many patients are surprised to learn that pigmentation can worsen indoors. Visible light exposure from sunlight through windows and digital screens plays a real role, especially in melasma and brown skin.”
This article explains the science behind visible light pigmentation, how it differs from UV and heat, and what actually helps protect the skin.
What Is Visible Light and Blue Light?
Visible light makes up about 50% of the sunlight spectrum. Unlike UV radiation, visible light:
- Is not blocked by standard sunscreens
- Penetrates glass windows
- Is present indoors
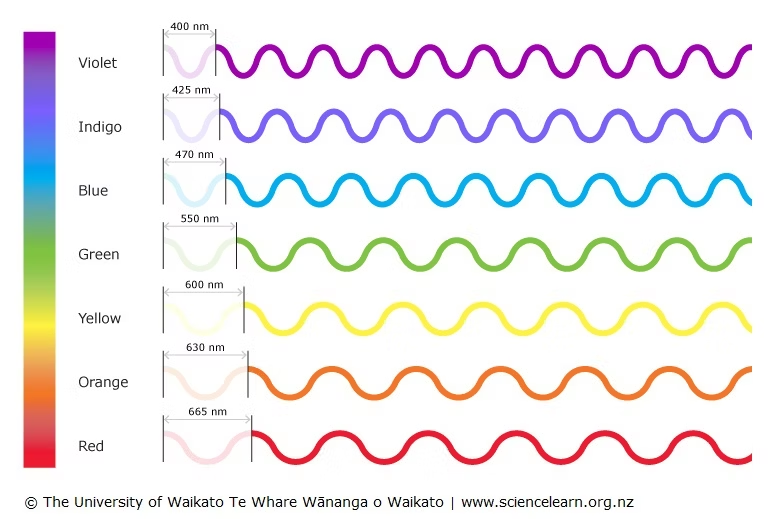
Blue light is a subset of visible light with shorter wavelengths and higher energy. It comes from:
- Sunlight
- Phone screens
- Laptops
- Tablets
- LED lighting
While blue light exposure from screens is lower than sunlight, cumulative daily exposure matters, especially for pigment-prone skin.
Visible light is a major reason for melasma not improving, especially in individuals with darker skin tones.
How Visible Light Triggers Pigmentation
Visible light affects pigmentation through different biological pathways than UV radiation.
1. Activation of Melanocytes via Opsin Receptors
Research shows that melanocytes contain opsin-3 receptors, which respond specifically to visible light. Why melasma keeps coming back? It is largely due to ongoing triggers such as sun and visible light exposure, hormonal fluctuations, heat, and inflammation, which continue to stimulate excess melanin production even after treatment. How inflammation triggers PIH lies in the skin’s response to injury or irritation, where inflammatory signals overstimulate melanocytes, leading to excess melanin deposition and lingering dark marks after the skin heals.
When exposed:
- Melanocytes increase melanin production
- Pigment darkens without UV damage
- The response is stronger in darker skin tones
This explains why pigmentation can worsen even without sunburn or tanning.
“Visible light doesn’t damage DNA the way UV does, but it still signals melanocytes to produce pigment. This makes it particularly relevant for melasma and PIH,” says Dr. Faiza Shams.
2. Stronger Effect in Deeper Skin Tones
Multiple studies show that visible light causes:
- Minimal pigment change in lighter skin
- Significant and long-lasting pigmentation in brown and deeper skin tones
This is why visible light protection is now considered essential in pigmentation management for Indian and Asian skin.
3. Synergy With Heat and Inflammation
Visible light rarely acts alone.
It amplifies:
- Heat-induced inflammation
- Vascular signaling in melasma
- Post-inflammatory pigment pathways
This synergy explains why pigmentation worsens indoors during summer even without direct sun exposure.
Blue Light From Screens: Does It Really Matter?
Blue light from screens is weaker than sunlight, but chronic exposure adds up.
Key considerations:
- Prolonged daily exposure
- Close proximity to screens
- Already active pigmentation disorders
In pigment-prone individuals, blue light contributes to:
- Persistent dullness
- Worsening melasma patches
- Slower pigment fading
“Screens alone may not cause pigmentation, but in someone with melasma or PIH, they can slow recovery and contribute to relapse,” explains Dr. Faiza Shams.
Why Sunscreen Alone Fails Indoors
Many patients feel their pigmentation is not improving despite sunscreen, but standard sunscreens do not protect against visible light. Most sunscreens are designed to block:
- UVB
- UVA
They do not block visible light.

This is why pigmentation may worsen:
- Near windows
- While driving
- Indoors with natural daylight
Without visible light protection, melanocytes remain stimulated.
Iron Oxides: The Missing Piece in Pigmentation Protection
Iron oxides are pigments added to tinted mineral sunscreens.
They:
- Reflect and absorb visible light
- Reduce blue light penetration
- Improve melasma outcomes
Understanding how to fix pigmentation that is not improving requires using sunscreen that protects against visible light, such as iron oxide formulas.
“For patients with melasma or persistent hyperpigmentation, I almost always recommend tinted sunscreens with iron oxides,” says Dr. Faiza Shams.
Visible Light vs UV vs Heat: How They Differ
| Trigger | Requires Sun | Acts Indoors | Blocks by Sunscreen | Pigment Risk |
|---|---|---|---|---|
| UV | Yes | Limited | Yes | High |
| Heat | No | Yes | No | High |
| Visible Light | No | Yes | No (unless tinted) | High |
This explains why comprehensive pigment control must address all three.
Who Is Most Affected by Visible Light Pigmentation?
Visible light has a stronger impact on:
- Melasma-prone individuals
- PIH-prone skin
- Indian and Asian skin tones
- People near windows daily
- Those using aggressive actives
Visible light can worsen pigmentation, especially in deeper skin tones, because why visible light affects brown skin more is linked to higher melanin content that absorbs visible light energy and stimulates melanocytes to produce even more pigment.
How to Protect Skin From Visible and Blue Light
1. Use Tinted Mineral Sunscreen Daily
Look for:
- Broad-spectrum SPF 30–50
- Iron oxides listed in ingredients
- Mineral filters (zinc oxide, titanium dioxide)
Apply even when staying indoors near windows.
2. Reduce Inflammation First
Visible light worsens pigment most in inflamed skin.
Use calming ingredients:
- Niacinamide
- Azelaic acid
- Tranexamic acid
- Ceramides
Inflamed skin reacts more strongly to visible light.
3. Adjust Screen Habits (When Possible)
- Increase screen distance
- Use screen filters
- Avoid unnecessary prolonged exposure
This supports pigment recovery but does not replace skincare protection.
4. Avoid Over-Treatment
Over-exfoliation increases sensitivity to visible light.
“Barrier-damaged skin reacts more aggressively to visible light. Calming the skin often improves pigmentation more than adding stronger actives,” notes Dr. Faiza Shams.
Does Visible Light–Induced Pigmentation Fade?
Yes—but only when:
- Visible light exposure is reduced
- Iron oxide protection is used
- Inflammation is controlled
Without these steps, pigmentation often plateaus or relapses.
Science-Backed Insights You Should Know
Recent dermatology research confirms:
- Visible light activates melanocytes independently
- Opsin receptors play a role in pigment signaling
- Iron oxides significantly reduce pigmentation worsening
- Deeper skin tones are more affected
- Indoor exposure matters clinically
These findings explain why many patients plateau despite “correct” routines.
Final Thoughts
Pigmentation does not only respond to the sun.
It responds to light, heat, inflammation, and skin biology.
Visible light and blue light are silent contributors that keep pigmentation active indoors. Once addressed—alongside UV and heat—pigment disorders become far more manageable. If your pigmentation is not improving, visible light exposure may be the missing factor in your routine.
As Dr. Faiza Shams summarizes:
“Understanding visible light has changed how we manage pigmentation. It explains why some patients struggle despite excellent sun protection.”
References
- Passeron T. et al., “Visible Light and Melanogenesis in Skin of Color,” Journal of the European Academy of Dermatology, 2022–2024.
- Mahmoud B.H. et al., “Role of Visible Light in Melasma,” Journal of Investigative Dermatology, 2021–2023.
- Grimes P.E., “Pigmentation Disorders and Visible Light Exposure,” Dermatologic Clinics, 2022–2024.
FAQS
1. Can visible light really cause pigmentation without sun exposure?
Yes. Dermatology research shows that visible light can activate melanocytes through specific receptors in the skin, leading to pigmentation even without UV exposure. This effect is stronger in melasma-prone and deeper skin tones.
2. Does blue light from phone and laptop screens worsen melasma?
Blue light from screens is weaker than sunlight, but long-term daily exposure can contribute to melasma worsening, especially in people with existing pigmentation. It can slow pigment fading and increase the risk of recurrence.
3. Why does pigmentation worsen indoors even when I use sunscreen?
Most sunscreens protect against UV radiation but do not block visible light. Indoor daylight and screens emit visible light that can still stimulate melanin production unless iron-oxide tinted sunscreens are used.
4. What is the best protection against visible light–induced pigmentation?
The most effective protection is a tinted mineral sunscreen containing iron oxides. These pigments help block visible and blue light and have been shown to reduce pigmentation worsening, especially in melasma.
5. Who is most at risk for visible light–induced hyperpigmentation?
People with melasma, post-inflammatory hyperpigmentation (PIH), Indian or Asian skin tones, and those who spend long hours indoors near windows or screens are most susceptible to visible light–induced pigmentation.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810