Inflammation-Induced Pigmentation: How Low-Grade Skin Inflammation Triggers Dark Spots
Table of Contents
Introduction: When Pigmentation Isn’t Caused by Sun Alone
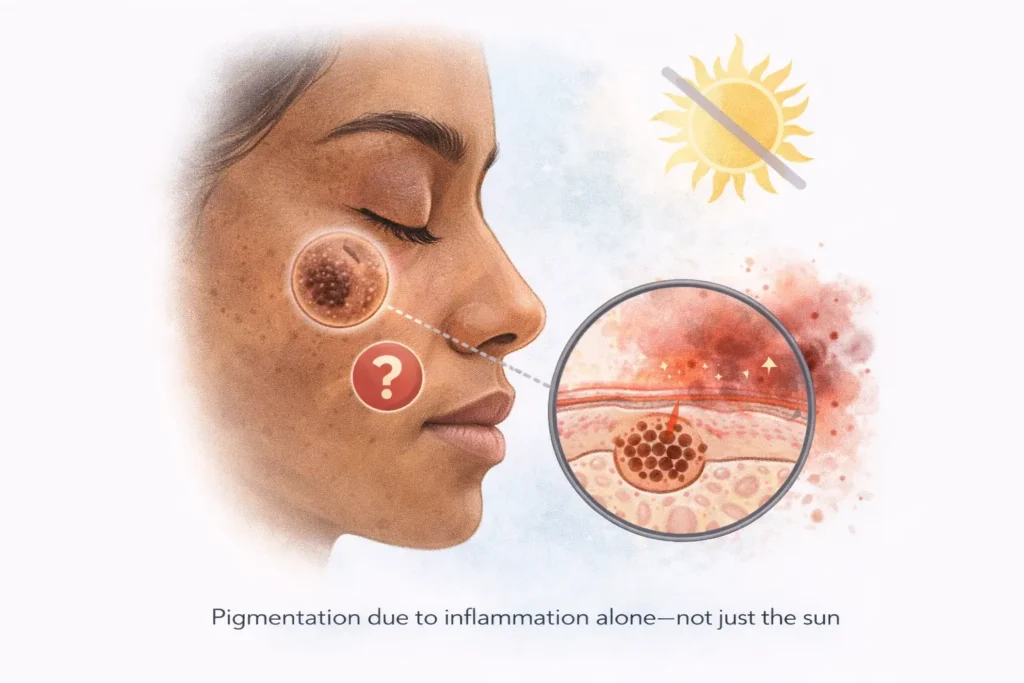
Many people associate dark spots with sun exposure or acne marks.
Yet pigmentation often appears—or worsens—even without obvious injury, breakouts, or tanning.
This happens because inflammation alone can trigger pigmentation.
Inflammation-induced pigmentation is one of the most overlooked mechanisms behind melasma relapse, stubborn uneven tone, and treatment resistance. Understanding it explains why gentle-looking routines still lead to darkening—and why pigmentation sometimes worsens before it improves.
What Is Inflammation-Induced Pigmentation?
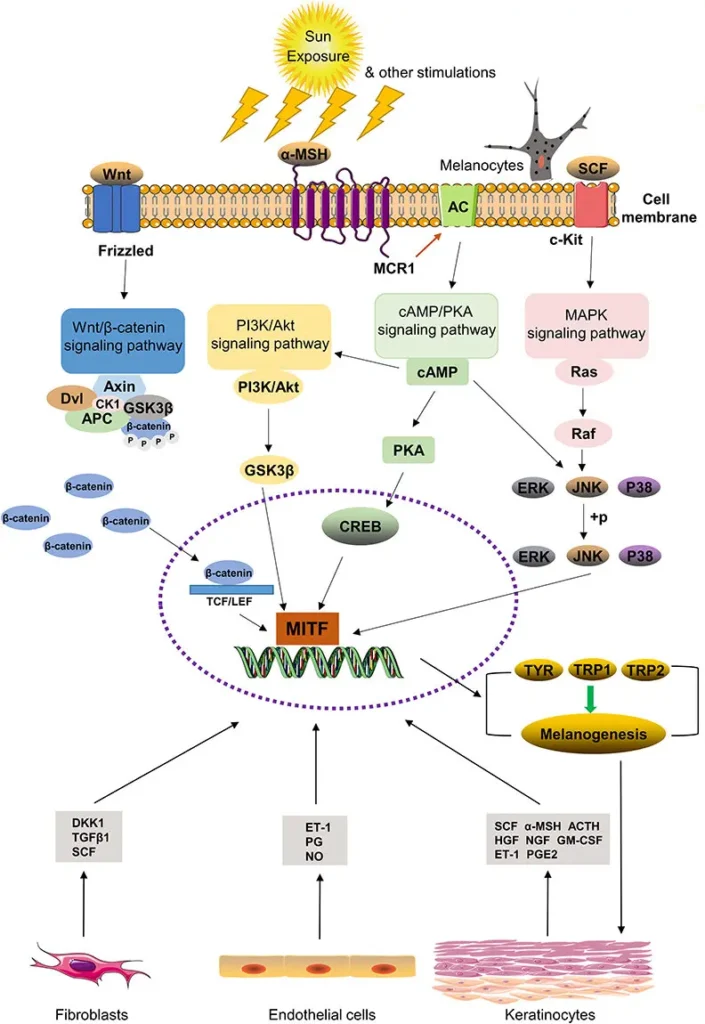
Inflammation-induced pigmentation refers to melanin overproduction triggered by inflammatory signals, not by direct pigment stimulation alone.
Managing inflammation with serums for sensitive and reactive skin can support long-term improvement.
Unlike classic post-inflammatory hyperpigmentation (PIH), this process can occur with:
- No visible injury
- No acne or rash
- No peeling or wounds
The inflammation is subclinical—low-grade, persistent, and often invisible.
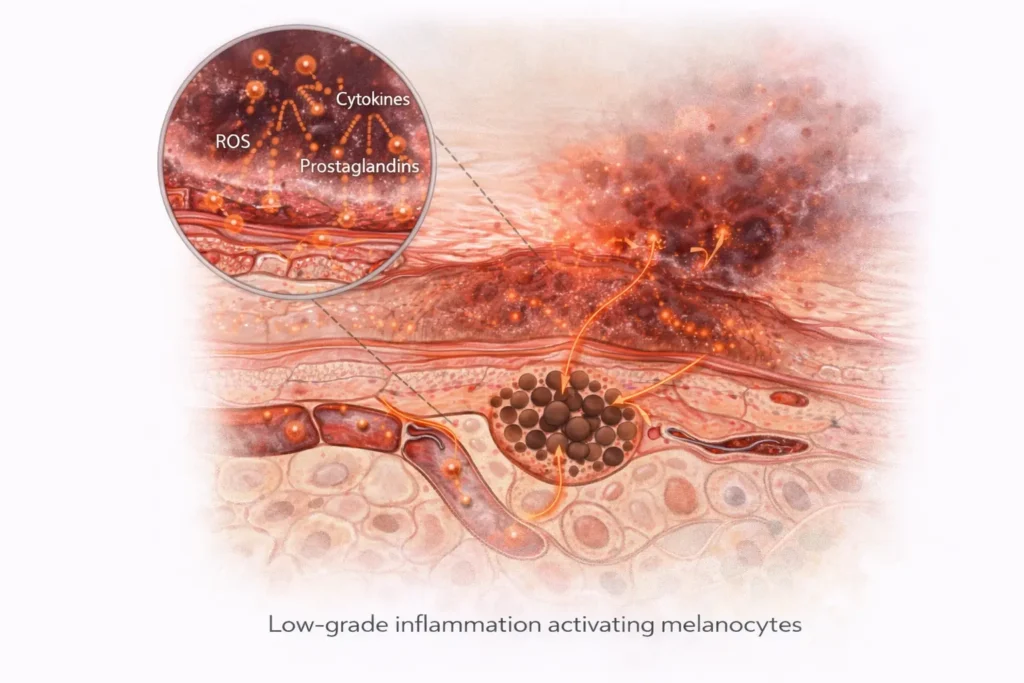
How Low-Grade Inflammation Activates Melanocytes
Melanocytes are highly sensitive cells.
They respond not only to UV light, but also to chemical and immune signals released during inflammation.
Low-grade inflammation releases mediators such as:
- Cytokines
- Prostaglandins
- Reactive oxygen species
These signals:
- Increase melanocyte activity
- Enhance melanin synthesis
- Promote melanin transfer to surrounding cells
According to Dr. Faiza Shams:
“Inflammation does not need to be severe to cause pigmentation. In melasma-prone skin, even subtle inflammatory signaling can activate melanocytes and sustain darkening.”
Common Triggers of Inflammation-Induced Pigmentation
Barrier Disruption
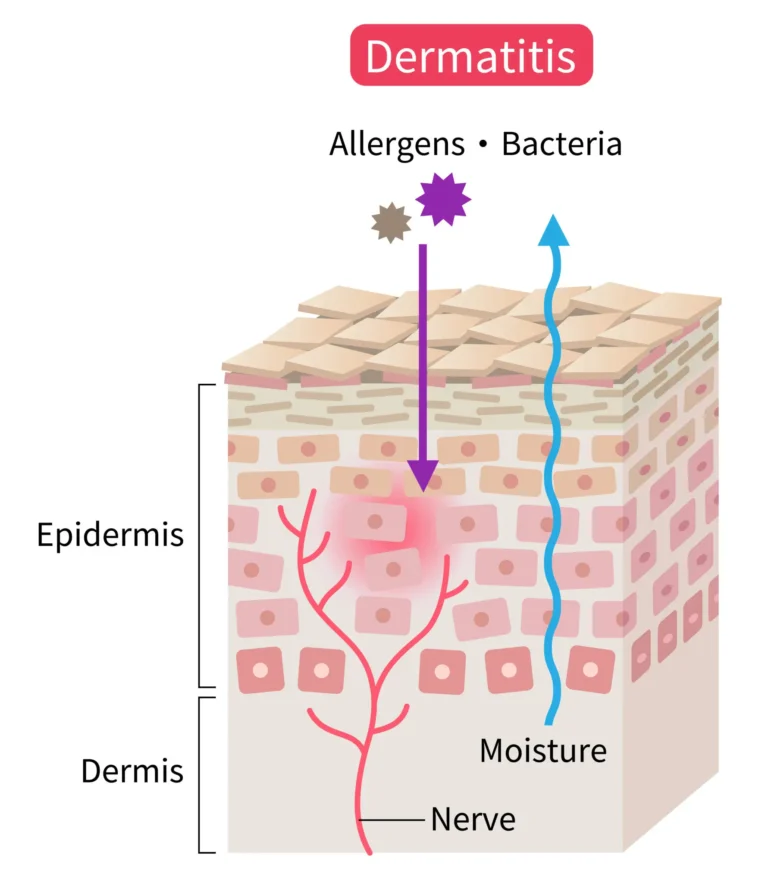
A compromised skin barrier allows irritants to penetrate more easily, maintaining a constant inflammatory state.
Skin barrier damage allows irritants, allergens, and microbes to penetrate more easily, increasing inflammation in the skin and triggering melanocytes to produce excess pigment as part of the skin’s defensive response.
Overuse of Actives
Frequent exfoliation, strong retinoids, or multiple actives layered together often create irritation that is not always visible—but biologically active.
Heat and Friction
Heat exposure, rubbing, and mechanical stress increase inflammatory mediators, particularly in melasma-prone skin.
Inappropriate “Brightening” Products
Products designed to fade pigment can paradoxically worsen it if they trigger inflammation.
Why Inflammation-Induced Pigmentation Persists
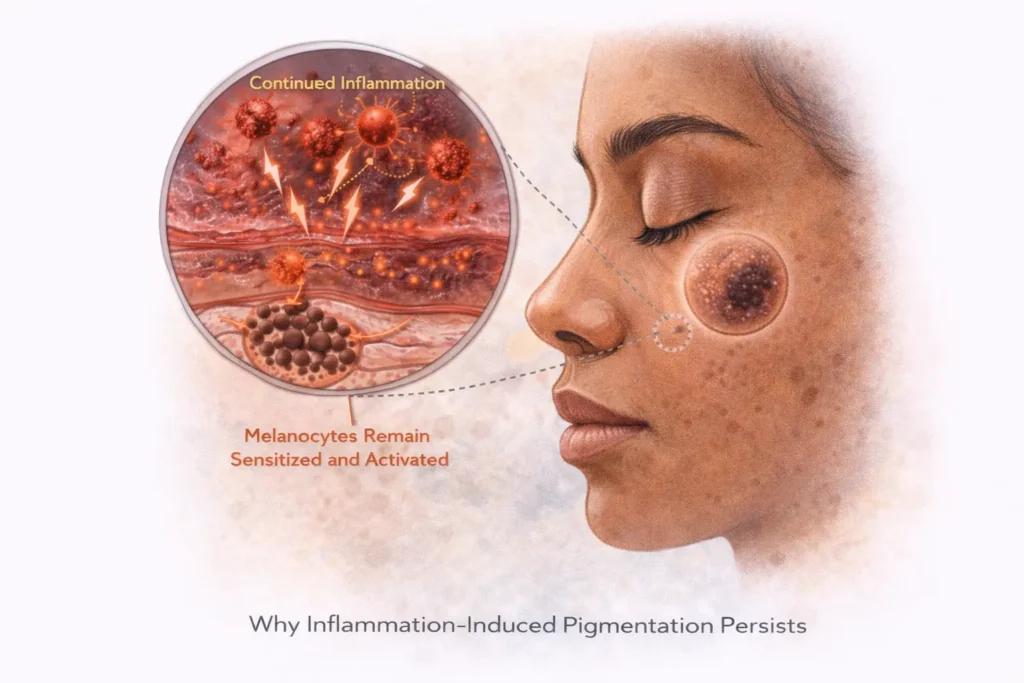
One of the most frustrating aspects of this type of pigmentation is persistence.
Even after the visible trigger is removed:
- Inflammatory signaling may continue
- Melanocytes remain sensitized
- Pigment production stays elevated
Dr. Faiza Shams explains:
“Once melanocytes are repeatedly activated by inflammation, they enter a reactive state. Without calming the skin, pigmentation control becomes unstable.”
This explains why pigmentation returns quickly after stopping treatment.
Inflammation-Induced Pigmentation vs Post-Inflammatory Hyperpigmentation
While related, these are not identical.
| Feature | Inflammation-Induced Pigmentation | PIH |
|---|---|---|
| Visible injury | Often absent | Usually present |
| Inflammation level | Low-grade, chronic | Acute |
| Duration | Persistent | Gradual fading |
| Common in melasma | Very common | Variable |
| Trigger | Barrier stress, irritation | Acne, wounds |
Understanding this difference is critical for choosing the right management approach.
Why Traditional Pigmentation Treatments Often Fail
Many pigmentation treatments focus solely on:
- Blocking melanin synthesis
- Increasing exfoliation
- Speeding cell turnover
If inflammation is not addressed, these approaches can:
- Increase irritation
- Prolong melanocyte activation
- Worsen long-term outcomes
This is why some treatments work initially but fail to maintain results.
How to Control Inflammation-Induced Pigmentation Safely
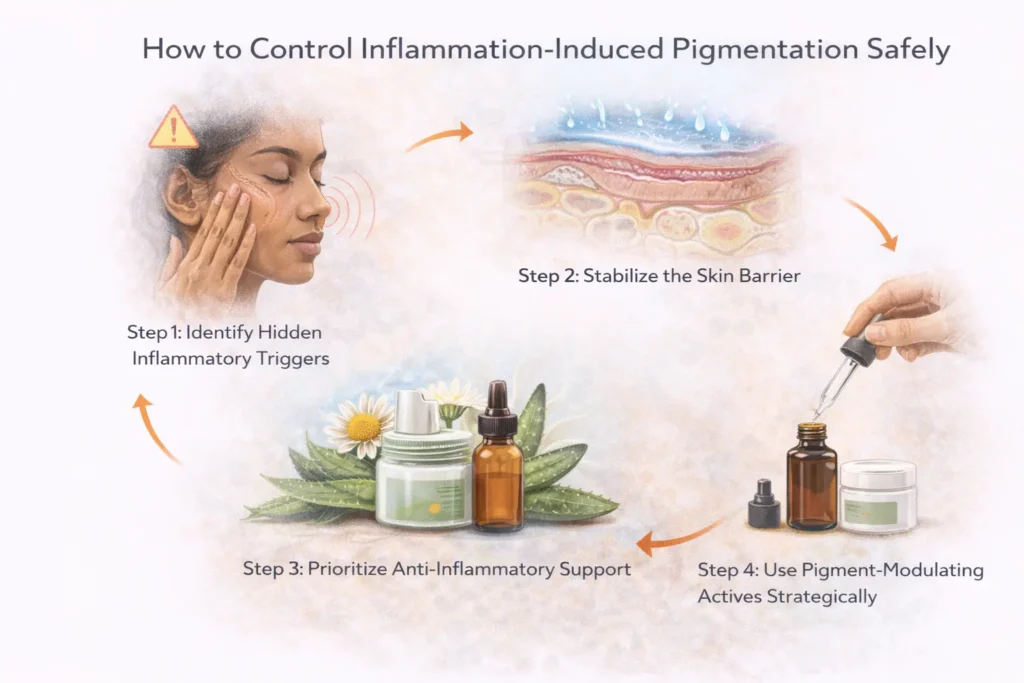
Step 1: Identify Hidden Inflammatory Triggers
Stinging, warmth, tightness, or redness after skincare are early signs—even if pigmentation hasn’t changed yet.
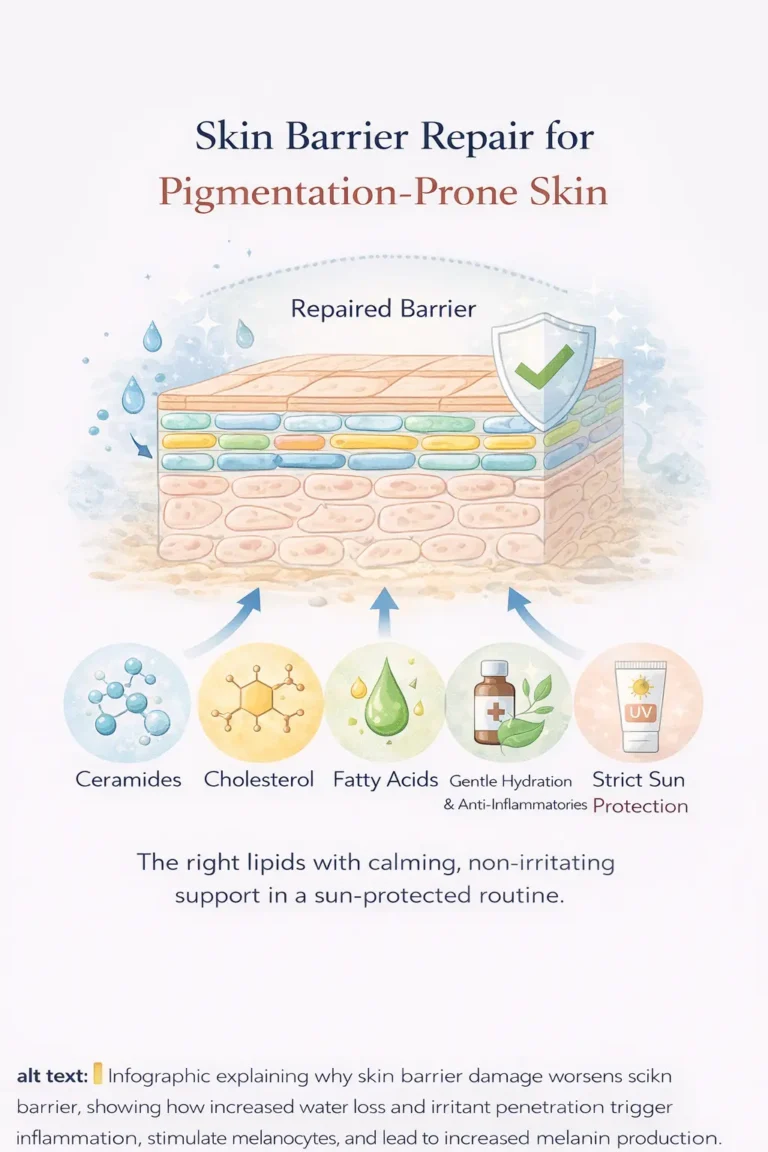
Step 2: Stabilize the Skin Barrier
A stable barrier reduces inflammatory signaling and limits irritant penetration.
Repairing the skin barrier in pigmentation-prone skin is essential because a stronger, healthier barrier reduces ongoing inflammation and helps prevent repeated melanin overproduction that leads to stubborn dark spots.
Step 3: Prioritize Anti-Inflammatory Support
Calming the skin lowers melanocyte stimulation more effectively than aggressive brightening.
Step 4: Use Pigment-Modulating Actives Strategically
Actives should be introduced only after inflammation is controlled—not during active irritation.
Why Calming the Skin Often Improves Pigmentation First
Many patients notice:
- Less redness
- Fewer flare-ups
- Stabilization of dark spots
before actual fading begins.
This is expected.
Reducing inflammation prevents new pigment formation, creating the conditions necessary for existing pigmentation to fade gradually.
Learn about why pigmentation looks darker before it improves?
Signs Your Inflammation-Driven Pigmentation Is Improving
Positive indicators include:
- Reduced sensitivity to products
- Less warmth or flushing
- Pigmentation stops spreading
- Improved tolerance to actives
Visible lightening usually follows later.
Long-Term Management of Inflammation-Induced Pigmentation
This type of pigmentation is best managed, not rushed.
Long-term stability requires:
- Ongoing barrier care
- Careful use of actives
- Consistent sun and light protection
- Avoidance of irritation cycles
Dr. Faiza Shams summarizes:
“In pigmentation-prone skin, controlling inflammation is not supportive care—it is central to pigment control.”
Final Thoughts: Treat Inflammation, Not Just Pigment
Inflammation-induced pigmentation explains why dark spots behave unpredictably and why many routines fail despite good intentions.
Pigment does not exist in isolation.
It reflects the skin’s inflammatory state.
When inflammation is reduced, melanocytes settle—and pigmentation becomes controllable again.
FAQS
1. Can pigmentation develop without acne or visible skin injury?
Yes. Persistent low-grade skin inflammation can activate melanocytes even without acne, wounds, or peeling, leading to gradual darkening and uneven skin tone.
2. Why does pigmentation worsen even when using gentle skincare products?
Pigmentation can worsen if the skin barrier is compromised, allowing mild products to trigger inflammation that stimulates melanin production in sensitive or pigmentation-prone skin.
3. Does calming the skin help reduce dark spots?
Yes. Reducing inflammation and stabilizing the skin barrier helps prevent new pigment formation and creates conditions for existing dark spots to fade more effectively over time.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810