Photodamage vs Pigmentation: How UV, Heat & Pollution Create Stubborn Dark Patches
Table of Contents
Introduction: Why Pigmentation Is No Longer Just a Melanin Problem
Pigmentation disorders are rising globally, despite better sunscreens, more advanced lasers, and an ever-expanding list of brightening ingredients. Patients today are more educated than ever. They use SPF daily. They avoid harsh products. They invest in treatments. Yet dark patches persist, deepen, or return.
This contradiction is frustrating for patients and clinicians alike.
If pigmentation were simply the result of excess melanin, treatment outcomes would be faster and more predictable. Lightening agents would work consistently. Procedures would provide lasting clearance. But in reality, pigmentation behaves more like a chronic condition than a cosmetic concern.
Many individuals notice that their pigmentation worsens even when they are indoors, even when they are not tanning, and even when they are doing “everything right.” This is where the traditional explanation of pigmentation begins to fail.
Pigmentation is not just about melanin. It is about why melanocytes are being repeatedly triggered. One of the most overlooked biological drivers behind this persistent stimulation is photodamage.
Understanding photodamage shifts the conversation from surface lightening to long-term skin health. It explains treatment failures, rebound pigmentation, and why prevention must extend beyond sunscreen alone.
Learn why pigmentation treatments fail?
What Is Photodamage? (And Why It’s Different From Sunburn)
Photodamage refers to cumulative, long-term skin injury caused by repeated exposure to ultraviolet radiation, visible light, infrared heat, and environmental pollutants. Unlike sunburn, which is an acute inflammatory response, photodamage develops gradually and often silently.
Sunburn is obvious. The skin turns red, feels painful, and eventually peels. Photodamage, on the other hand, accumulates at the cellular level over years. It alters DNA, disrupts collagen, destabilizes blood vessels, and keeps inflammatory pathways persistently active.
This chronic damage does not always show up as wrinkles or sagging, especially in darker skin tones. In pigmentation-prone skin, photodamage often manifests as brown, grey, or uneven patches rather than visible aging.
Photodamage is not the result of one bad sun exposure. It is the biological memory of repeated exposure layered over time.
Photodamage vs Pigmentation: Understanding the Difference
Pigmentation refers to increased or uneven melanin production. Photodamage refers to the environmental injury that drives melanocytes into a hyper-reactive state.
Pigmentation is a symptom, not a disease. When treatment focuses only on breaking down pigment or suppressing tyrosinase, the deeper stimulus remains active. As a result, melanocytes continue to receive signals to produce melanin.
This is why pigmentation often fades temporarily and then returns. The pigment was reduced, but the underlying photodamage was never addressed.
A useful way to think about this is that pigmentation is the visible smoke, while photodamage is the fire underneath. Unless the fire is controlled, smoke will keep appearing.
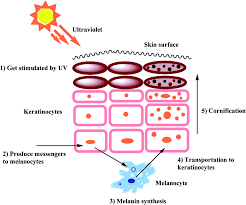
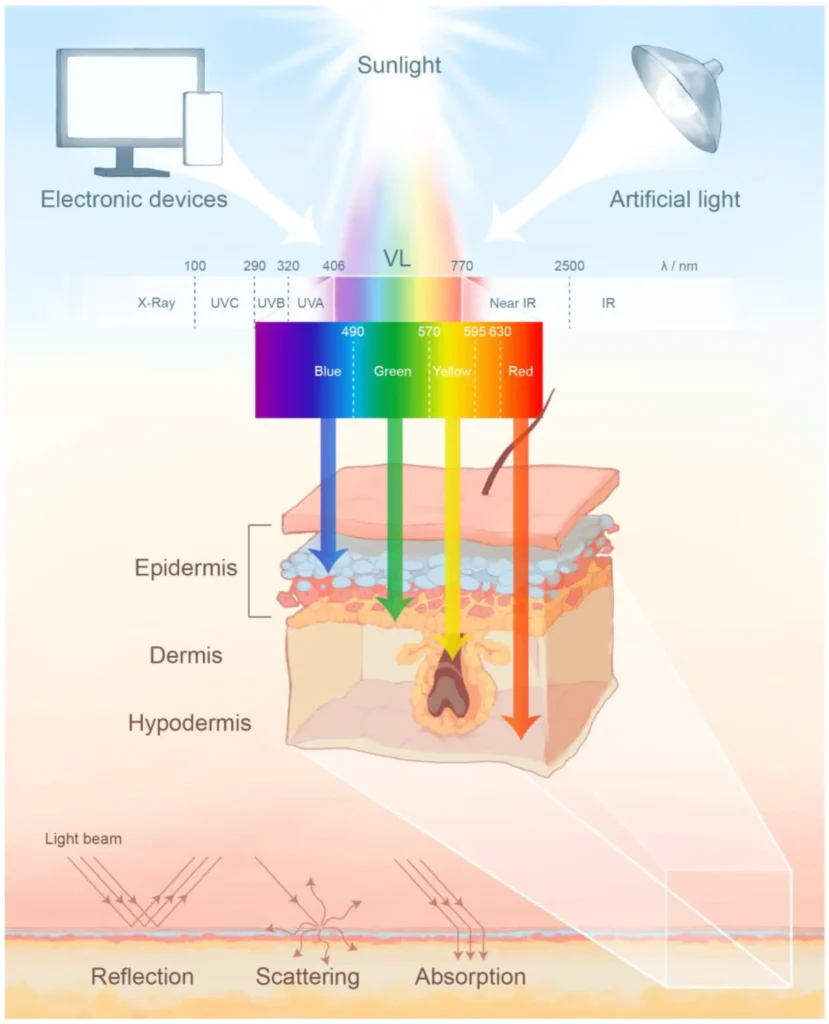
How UV Radiation Triggers Pigmentation at a Cellular Level
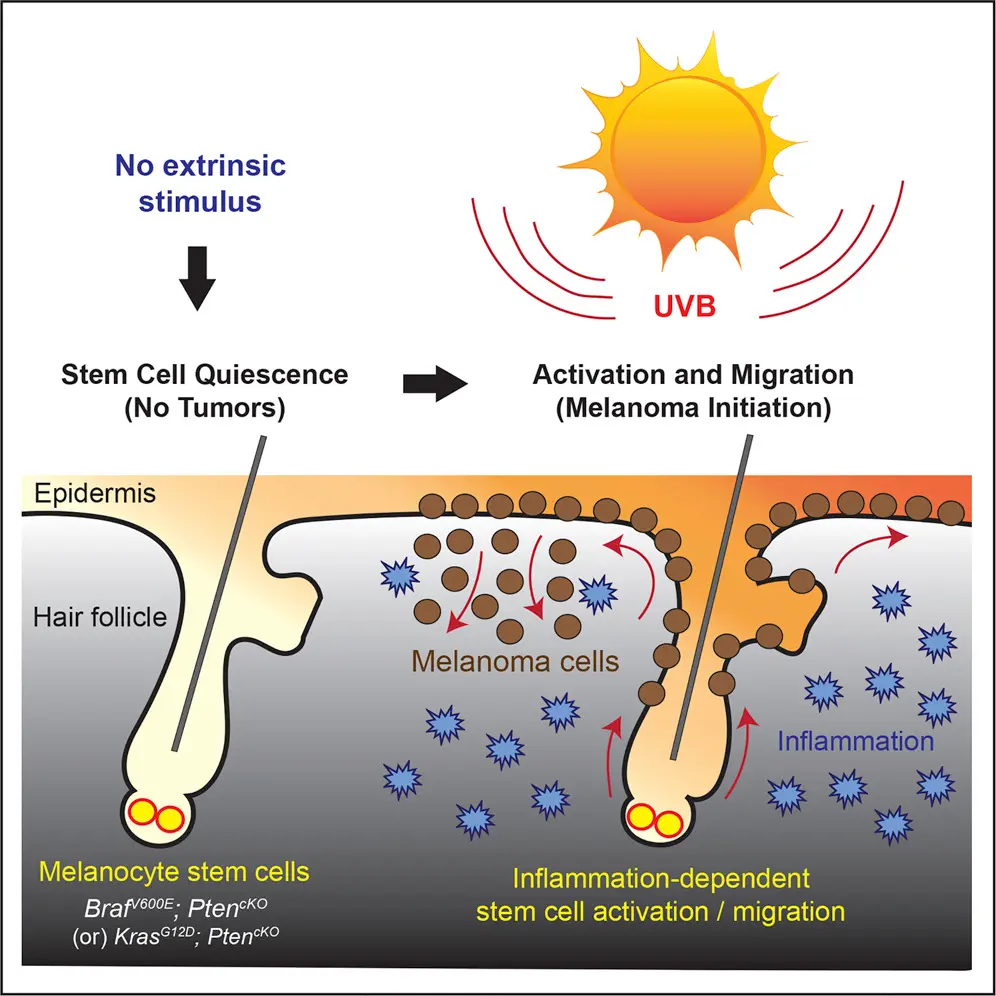
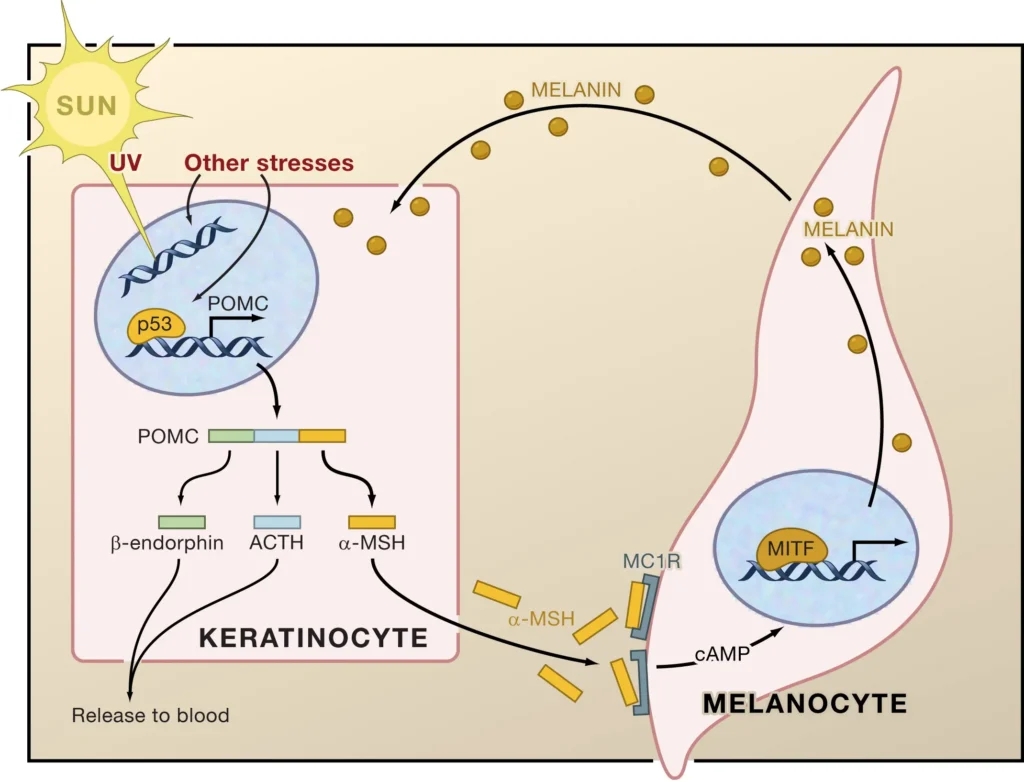
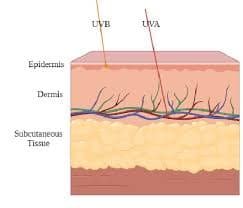
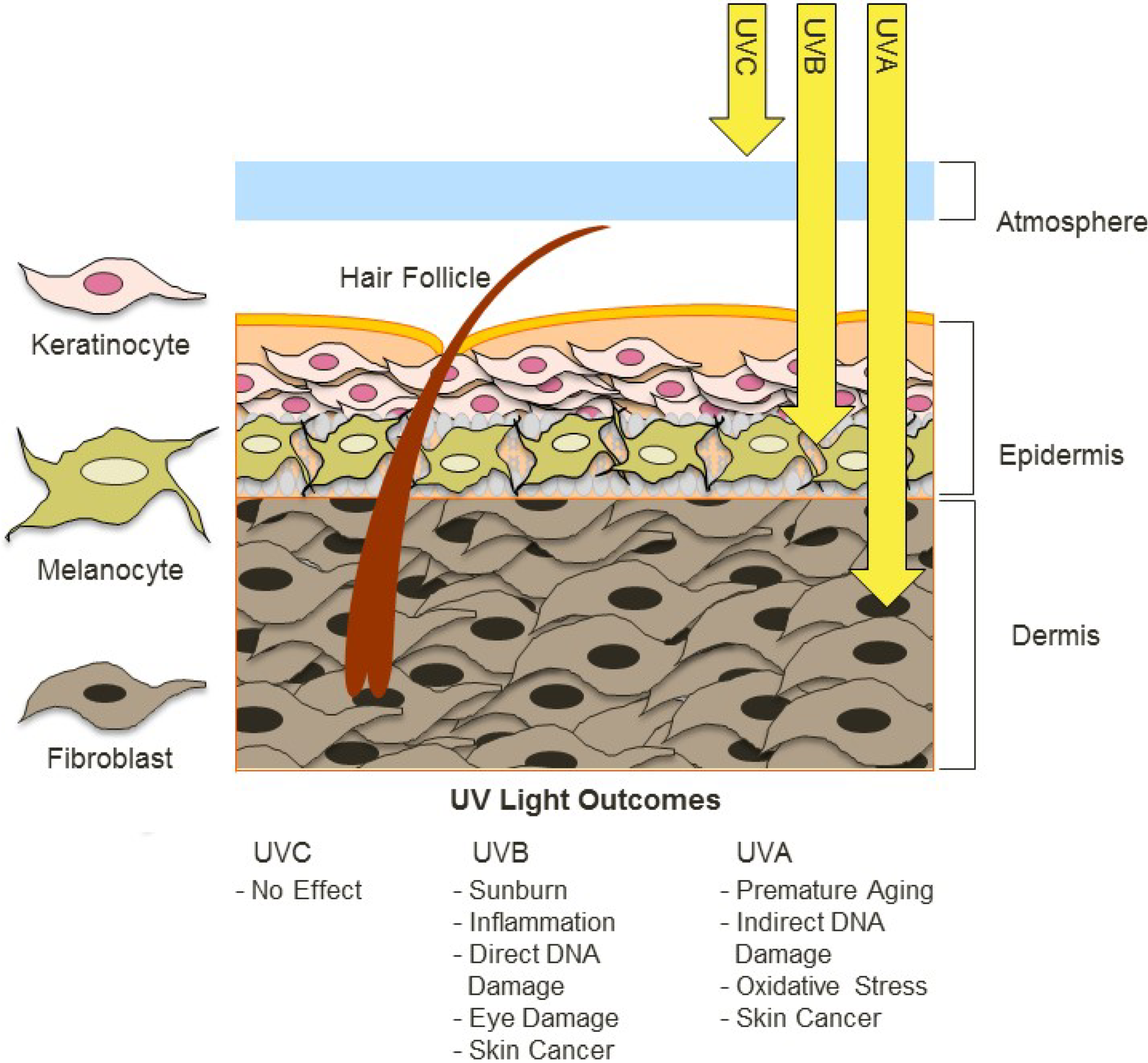
Ultraviolet radiation affects pigmentation through multiple overlapping pathways.
UVB rays primarily impact the epidermis. They cause direct DNA damage in keratinocytes, activating the p53 pathway. This leads to increased production of melanocyte-stimulating signals as a protective response. Melanin is produced not for cosmetic reasons, but as a defense mechanism.
UVA rays penetrate deeper into the dermis. They damage fibroblasts, blood vessels, and the extracellular matrix. This damage triggers inflammatory mediators that indirectly stimulate melanocytes from below.
Repeated UV exposure trains melanocytes to remain active even when exposure is minimal. Over time, this leads to persistent pigmentation patterns, particularly on sun-exposed areas of the face.
This explains why pigmentation can continue to worsen even without visible sunburn or tanning.
According to Dr. Faiza Shams, “When patients think pigmentation is only a surface issue, they underestimate how deeply UV exposure rewires melanocyte behavior. Once that signaling loop is established, lightening alone is never enough.”
- UVA vs UVB effects on melanocytes
- DNA damage and p53 activation
- Persistent melanocyte stimulation
The Role of Heat in Deepening Pigmentation
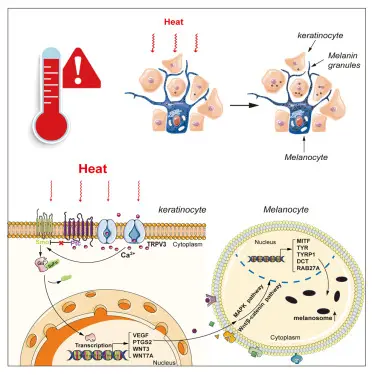
Heat is one of the most underestimated contributors to pigmentation.
Infrared radiation from sunlight, hot climates, cooking environments, exercise, and even indoor heat sources activates vascular and inflammatory pathways in the skin. Heat increases blood flow, dilates vessels, and enhances inflammatory signaling.
Unlike UV exposure, heat does not immediately darken the skin. This makes it easy to overlook. However, heat amplifies melanocyte activity and worsens existing pigmentation over time.
Many patients report that their pigmentation worsens in summer despite diligent sunscreen use. In these cases, heat—not UV alone—is often the missing factor.
Pollution, Oxidative Stress, and Dark Patches
Environmental pollution contributes significantly to photodamage through oxidative stress.
Pollutants generate free radicals that overwhelm the skin’s natural antioxidant defenses. These reactive molecules damage cell membranes, proteins, and DNA. They also disrupt normal melanin distribution, causing pigment to become more uneven and persistent.
Growing evidence highlights pollution as a major contributor to photodamage-induced pigmentation. A 2023 multicenter study published in Environmental Dermatology linked particulate matter exposure to increased tyrosinase activity and uneven melanin distribution, particularly in urban populations. In 2025, researchers further confirmed that oxidative stress from pollutants weakens the epidermal barrier, increasing pigment persistence and treatment resistance.
Dr. Faiza Shams explains, “In highly polluted environments, pigmentation behaves more aggressively. Even excellent skincare fails if oxidative stress and barrier damage are not addressed simultaneously.”
- Free radical generation
- Barrier disruption and melanin leakage
- Urban pigmentation patterns
Pollution further weakens the skin barrier, allowing irritants and inflammatory triggers to penetrate more deeply. In pigmentation-prone skin, this creates a perfect environment for chronic melanocyte stimulation.
Urban populations consistently show higher rates of treatment-resistant pigmentation, highlighting the role of environmental exposure beyond sunlight alone.
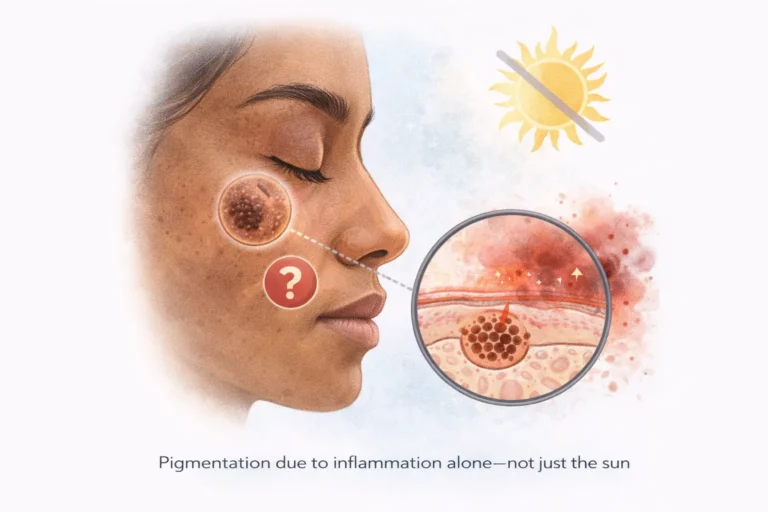
Inflammation: The Bridge Between Photodamage and Pigmentation
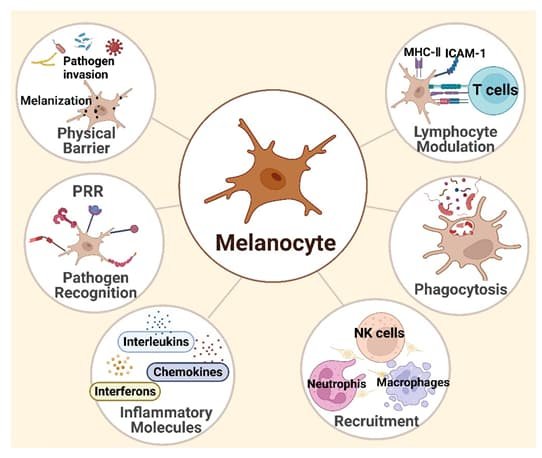
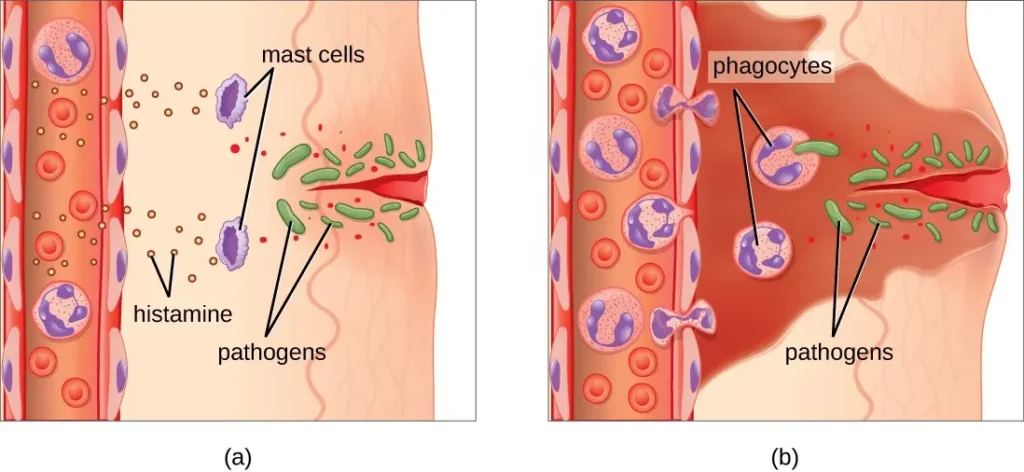
Inflammation is the central link connecting UV radiation, heat, pollution, and pigmentation.
Photodamage keeps the skin in a state of chronic low-grade inflammation. Cytokines, prostaglandins, and mast cells continuously signal melanocytes to remain active.
This ongoing inflammatory environment explains why pigmentation often coexists with sensitivity, burning, or stinging—even when the skin does not appear visibly inflamed.
Until inflammation is controlled, melanocyte activity remains heightened, and pigmentation remains difficult to treat.
Melanocyte Memory and Recurrent Pigmentation
Repeated photodamage alters melanocyte behavior at a genetic and epigenetic level. This phenomenon is often referred to as melanocyte memory.
Once melanocytes have been repeatedly stimulated, they become primed to respond aggressively to even minor triggers. This explains why pigmentation tends to recur in the same locations after treatment.
The concept of melanocyte memory has gained strong scientific support in recent years. A 2024 epigenetic analysis published in Experimental Dermatology demonstrated that melanocytes exposed to repeated photodamage undergo lasting genetic modulation, making them hyper-responsive to future triggers. This explains why pigmentation often returns in the same areas even after successful clearance.
Even when pigment appears cleared, melanocytes retain this heightened responsiveness. Without addressing photodamage, relapse becomes likely rather than exceptional.
As Dr. Faiza Shams notes, “Recurrent pigmentation is not a failure of treatment—it is evidence that melanocytes remember past damage. Without controlling photodamage, relapse is biologically expected.”
Why Brown and Asian Skin Is More Vulnerable to Photodamage
Darker skin tones contain more active melanocytes. While this provides some natural UV protection, it also increases the risk of pigmentation disorders.
Melanin itself can contribute to oxidative stress when overstimulated. Additionally, pigment clearance is slower in brown and Asian skin, allowing dark patches to persist longer.
Environmental exposure, cultural sun habits, and hotter climates further increase cumulative photodamage in these populations.
This combination explains why pigmentation disorders are more prevalent, more persistent, and more prone to relapse in skin of color.
Why Sunscreen Alone Is Not Enough
Sunscreen is essential, but it is not a complete solution.
Although sunscreen remains essential, recent literature emphasizes its limitations. A 2023 consensus paper in Photodermatology, Photoimmunology & Photomedicine highlighted that standard SPF testing does not account for visible light or infrared radiation, both of which contribute significantly to pigmentation in skin of color.
Dr. Faiza Shams emphasizes, “Sunscreen is necessary, but it is not complete protection. Patients with pigmentation must think beyond SPF and address heat, light, and environmental exposure as a whole.”
- Limitations of SPF
- Visible light and heat exposure
- False sense of protection
Most sunscreens primarily protect against UVB and part of the UVA spectrum. Many do not adequately shield against visible light or infrared heat. This creates a false sense of security.
Learn about iron oxide–based sunscreens.
Patients believe they are protected, yet photodamage continues through pathways that SPF does not fully address.
True pigmentation prevention requires broader environmental protection strategies, not SPF alone.
The Role of Skin Barrier Damage in Photodamage-Induced Pigmentation
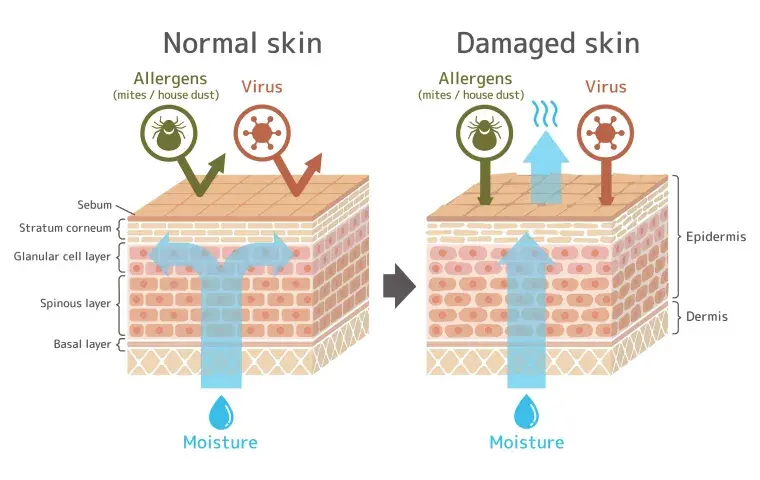
A compromised skin barrier amplifies photodamage.
Barrier disruption increases transepidermal water loss, triggers inflammation, and allows pollutants to penetrate more deeply. This prolongs recovery from environmental stress and worsens pigmentation.
Without barrier repair, even the best pigmentation treatments become less effective and more irritating.
Barrier health is not optional in pigmentation management—it is foundational.
Why Brightening Products Often Worsen Photodamage
Many brightening products rely on acids, exfoliants, or aggressive actives. While these may temporarily reduce surface pigment, they often thin the barrier and increase photosensitivity.
Over time, this accelerates photodamage rather than correcting it. Patients experience burning, redness, and rebound pigmentation, often misinterpreted as “purging” or resistance.
True brightening should calm and protect the skin, not stress it further.
How to Treat Pigmentation Caused by Photodamage (Correctly)
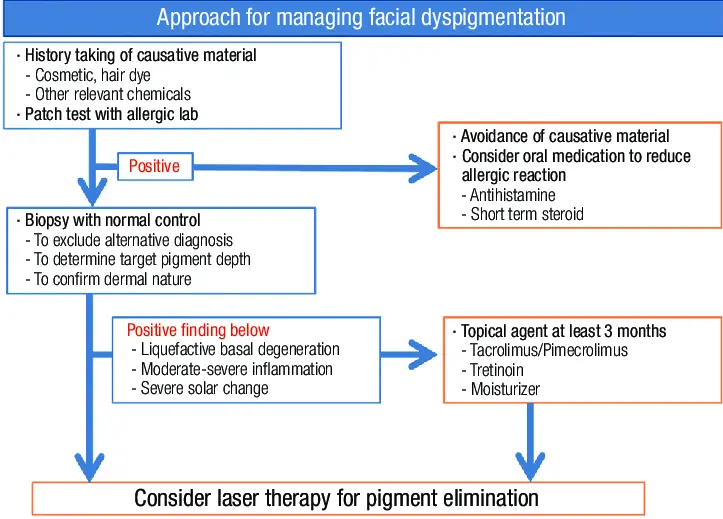
Effective treatment requires a shift in strategy:
Step 1: Stop ongoing photodamage
This includes broad-spectrum UV protection, visible light shielding, heat awareness, and pollution defense.
Step 2: Calm inflammation
Reducing inflammatory signaling is essential before aggressively targeting pigment.
Step 3: Repair the skin barrier
A resilient barrier improves tolerance, recovery, and treatment outcomes.
Step 4: Regulate melanocyte activity gently
Melanocytes should be normalized, not suppressed aggressively.
If you are ready to start a Vitamin C routine for dark spots, read our step-by-step guide on how to use Vitamin C Serum for hyperpigmentation on Pakistani skin.
Ingredients That Help Reverse Photodamage-Induced Pigmentation
Antioxidants help neutralize free radicals and reduce oxidative stress.
Evidence-based ingredient selection is critical. A 2024 review in Clinical, Cosmetic and Investigational Dermatology confirmed that antioxidants reduce oxidative stress–induced melanocyte activation, while barrier-repair formulations significantly improve treatment tolerance and long-term pigment stability.
Barrier-repair ingredients restore lipid balance and reduce inflammatory reactivity.
Anti-inflammatory agents calm melanocyte signaling without increasing sensitivity.
Ingredient selection matters less than formulation strategy and skin tolerance.
Dr. Faiza Shams advises, “The most effective pigmentation routines are not the strongest ones. They are the ones that lower inflammation, restore barrier resilience, and slowly normalize melanocyte behavior.”
- Antioxidants
- Barrier-repair actives
- Anti-inflammatory agents
Why Aggressive Procedures Can Backfire
Lasers and energy-based devices generate heat. In pigmentation-prone skin, this can worsen photodamage if not carefully managed.
Without proper skin preparation and patient selection, procedures increase the risk of rebound hyperpigmentation.
Aggressive treatments are not inherently bad, but timing, technique, and skin condition determine outcomes.
The Long-Term Strategy for Preventing Pigmentation Relapse
Long-term success depends on consistency rather than intensity.
Environmental protection, barrier maintenance, controlled use of actives, and lifestyle awareness all play critical roles.
Pigmentation management is ongoing, not episodic.
Final Thoughts: Treat the Damage, Not Just the Dark Spot
Pigmentation is not a surface flaw. It is a biological response to cumulative environmental injury.
When treatment focuses only on melanin, results remain temporary. When photodamage is addressed, pigmentation becomes more predictable, stable, and manageable.
Lasting pigmentation control begins by treating the damage beneath the surface—not just the dark spot itself.
FAQS
1. What is the difference between photodamage and pigmentation?
Photodamage refers to cumulative skin injury caused by repeated exposure to ultraviolet radiation, heat, visible light, and pollution. Pigmentation, on the other hand, is the visible result of this damage—appearing as dark patches or uneven skin tone. In other words, pigmentation is a symptom, while photodamage is the underlying biological trigger that keeps melanocytes overactive.
2. Why does pigmentation worsen even when I use sunscreen daily?
Sunscreen mainly protects against UVB and part of the UVA spectrum. It does not fully block visible light, infrared heat, or pollution-related oxidative stress—all of which contribute to photodamage. This is why pigmentation can worsen despite regular SPF use, especially in hot climates or urban environments.
3. Can photodamage cause pigmentation to keep coming back after treatment?
Yes. Repeated photodamage can create long-term changes in melanocyte behavior, often referred to as melanocyte memory. Even after successful treatment, these cells remain highly responsive to triggers like heat, light, or inflammation. Without addressing photodamage and barrier health, pigmentation relapse is biologically likely.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810