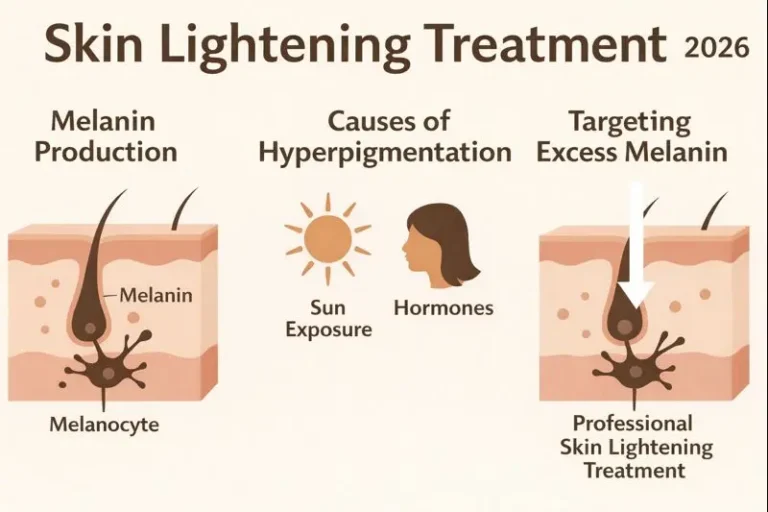
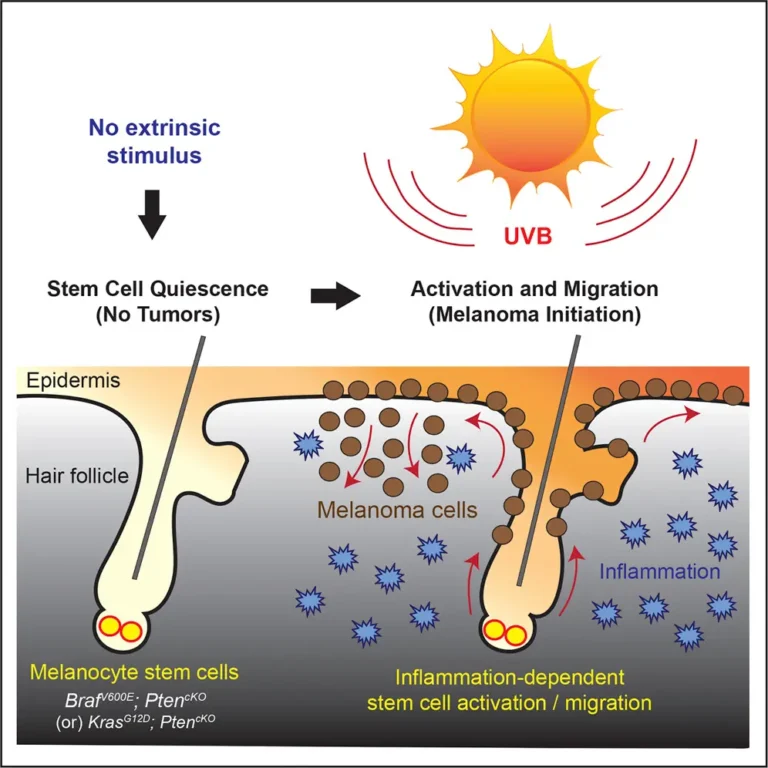
Exosomes for Pigmentation: Do They Really Work for Melasma and Dark Spots?
Table of Contents
Pigmentation is rarely simple.
Whether it is melasma, post-inflammatory hyperpigmentation, or stubborn dark spots that refuse to fade, most patients eventually realize something important: treating pigmentation is not just about “lightening” the skin.
It is about inflammation.
It is about cellular signaling.
It is about melanocyte memory.
To understand why pigmentation keeps recurring, read about melanocyte memory and recurrent pigmentation patterns.
In recent years, exosomes for pigmentation have entered the dermatology conversation as a next-generation regenerative treatment. Clinics now advertise exosome therapy for melasma, dark spots, and even post-laser pigmentation.
But do exosomes really work for hyperpigmentation?
Are they safe for skin of color?
And how strong is the scientific evidence?
Let’s examine the data — without hype.
Why Pigmentation Is So Difficult to Treat
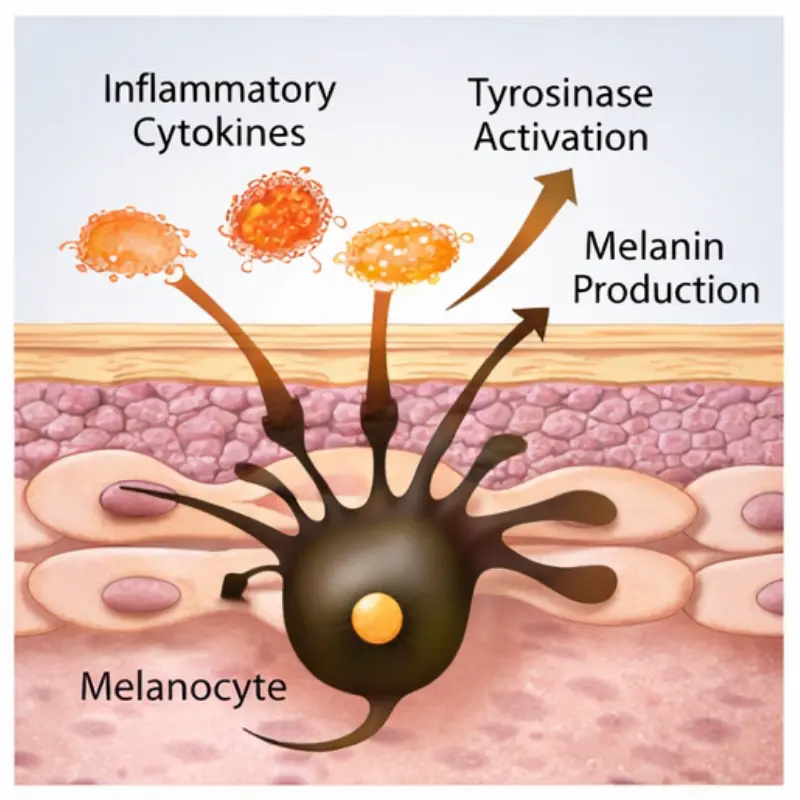
Before discussing exosomes, we need to understand why pigmentation keeps coming back.
Pigment disorders such as melasma and chronic hyperpigmentation involve:
- Overactive melanocytes
- Persistent inflammatory signaling
- Oxidative stress
- Barrier dysfunction
- UV and visible light triggers
- Heat-induced melanogenesis
If you’ve noticed that pigmentation improves slowly or plateaus, that is not accidental.
If you’ve ever wondered why pigmentation takes months to fade, understanding why pigmentation improves slowly over time can help set realistic expectations.
Many patients feel frustrated when their improvement suddenly stalls. Understanding why pigmentation treatment plateaus happen can help you adjust your strategy instead of abandoning treatment too early.
As I often explain to my patients:
“Pigmentation is rarely just about excess melanin. It is about inflammation, cellular memory, and barrier signaling. Exosomes target communication pathways, which makes them scientifically interesting — but they are not magic,” explains Dr. Faiza Shams.
This is where regenerative therapies enter the discussion.
What Are Exosomes in Dermatology?
Exosomes are tiny extracellular vesicles released by cells.
Think of them as microscopic communication packets. They carry:
- Proteins
- Lipids
- Growth factors
- MicroRNAs
- Anti-inflammatory mediators
Unlike stem cell therapy, exosomes are cell-free. They do not contain living cells. Instead, they carry signaling molecules that influence how other cells behave.
In dermatology, exosomes are being studied for:
- Skin rejuvenation
- Wound healing
- Hair restoration
- Acne scarring
- Hyperpigmentation
Exosomes fall under the umbrella of regenerative skincare science, where treatment focuses on improving cellular communication and repair instead of temporary cosmetic brightening.
How Exosomes May Help Hyperpigmentation
The potential benefit of exosomes for pigmentation lies in their ability to regulate signaling pathways.
1. Anti-Inflammatory Effects
Chronic micro-inflammation drives melanocyte activation.
This mechanism becomes especially important in inflammation-induced pigmentation, a condition where ongoing skin irritation keeps triggering melanin production.
Exosomes may reduce inflammatory cytokines that stimulate melanin production.
Less inflammation means fewer signals telling melanocytes to produce pigment.
2. Modulation of Melanogenesis
Preclinical research suggests exosomes may downregulate:
- Tyrosinase
- MITF pathways
- Melanin synthesis genes
This does not “bleach” skin. It regulates production.
That distinction matters.
3. Barrier Repair Support
Barrier dysfunction worsens pigmentation retention.
If your barrier is compromised, pigment lingers longer.
A compromised barrier significantly prolongs pigment persistence. Understanding skin barrier damage and repair mechanisms is essential when treating chronic hyperpigmentation.
Exosomes may accelerate keratinocyte repair and barrier recovery, indirectly improving pigment turnover.
4. Reduced Post-Procedure Pigmentation Risk
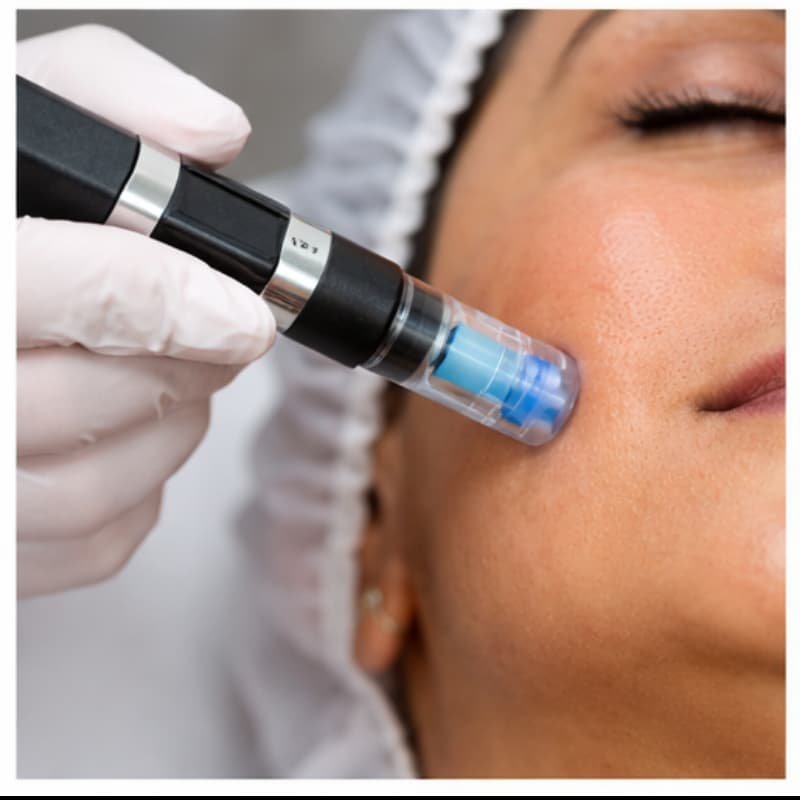
In darker skin types (Fitzpatrick IV–V), procedures can trigger post-inflammatory hyperpigmentation.
Exosomes used after microneedling or laser may reduce inflammatory downtime.
For patients considering combination treatments, reviewing microneedling before and after results for pigmentation-prone skin can help set realistic expectations.
What Does Current Research Say? (2022–2025 Evidence)
Scientific evidence for exosomes for melasma and hyperpigmentation is growing, but still limited.
Key findings from recent literature:
- Small pilot studies show improvement in melasma severity scores after exosome application.
- Preclinical studies demonstrate reduced melanogenesis signaling in vitro.
- Systematic reviews describe promising pigment reduction but emphasize the need for standardized protocols and larger randomized trials.
Important limitations:
- Small sample sizes
- Heterogeneous exosome sources
- Short follow-up duration
- Variable delivery methods
The evidence is promising — but not definitive.
This is not yet a first-line treatment.
Exosomes vs PRP for Pigmentation
Patients often ask whether exosomes are better than PRP.
Here is a simplified comparison:
Mechanism
PRP delivers platelet growth factors.
Exosomes deliver signaling RNA and regulatory molecules.
Inflammation Control
PRP can stimulate healing but may provoke inflammation.
Exosomes are thought to have stronger anti-inflammatory modulation.
Evidence Base
PRP has broader dermatologic literature.
Exosomes have newer, emerging data.
Regulation
PRP is autologous and widely accepted.
Exosome products vary in regulation depending on source.
At present, exosomes are not clearly superior to PRP. They are different tools.
Are Exosomes Safe for Skin of Color?
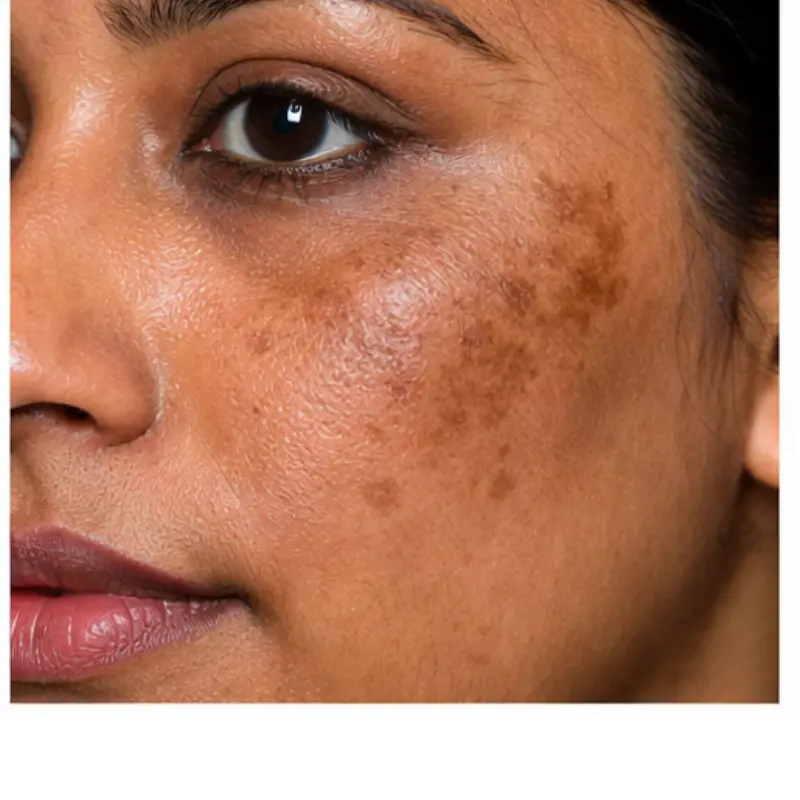
Safety is the most important question.
In patients with:
- Pakistani skin
- Indian skin
- Asian skin
Pigmentation risk is higher.
Pigmentation behaves differently in melanin-rich skin. If you want a deeper understanding of how hyperpigmentation presents in Indian skin types and broader patterns of Asian skin discoloration, these variations are important when choosing advanced treatments like exosomes.
Key safety considerations:
- Source of exosomes (human-derived vs synthetic vs plant-derived)
- Manufacturing standards
- Delivery method
- Risk of infection if injected
- Potential immune response
Injectable human-cell-derived exosomes have faced regulatory scrutiny internationally.
In my clinical practice, if exosomes are used, they are considered an adjunct — never a standalone replacement for evidence-based pigment protocols.
Who Is a Good Candidate for Exosome Therapy?
Exosome therapy for hyperpigmentation may be considered in:
- Resistant melasma
- Exosome therapy may be considered in patients experiencing recurrent pigmentation after stopping treatment, especially when conventional maintenance protocols fail to sustain results.
- Patients with barrier damage
- Post-laser inflammation cases
- Chronic inflammatory pigmentation
Not ideal candidates:
- Active infections
- Unrealistic expectations
- Very superficial, easily treatable pigment
What Results Can Patients Realistically Expect?
Exosomes are not bleaching agents.
Patients may notice:
- Improved skin texture
- Better glow
- Reduced inflammation
- Gradual softening of pigmentation
Pigment lightening, if it occurs, is slow.
“Exosomes should be seen as a regulatory therapy, not a bleaching treatment. Patients expecting overnight lightening will be disappointed,” says Dr. Faiza Shams.
For long-term success, strict photoprotection remains essential.
If you are not using iron oxide sunscreens for visible light protection, your pigmentation results are unlikely to sustain. Understanding how iron oxides work in skincare formulations is critical for long-term melasma control.
Are Exosomes the Future of Regenerative Pigmentation Treatment?
Possibly.
Regenerative dermatology is evolving rapidly.
But at this stage, exosomes are best viewed as:
An adjunct therapy.
A signaling modulator.
A recovery enhancer.
Not a miracle cure.
For most patients, proven pillars remain:
- Sunscreen
- Barrier repair
- Inflammation control
- Evidence-based actives
- Heat and visible light protection
Long-term pigmentation control is impossible without addressing visible light–induced pigmentation, especially in melanin-rich skin types.
Final Verdict: Should You Consider Exosomes for Pigmentation?
If you have:
- Resistant melasma
- Chronic inflammatory pigmentation
- Treatment plateau
- Recurrent pigment despite maintenance
Exosomes may be worth discussing with a qualified dermatologist.
However, they should only be used:
- With transparent sourcing
- With informed consent
- As part of a comprehensive pigmentation protocol
Pigmentation is complex.
There is no single silver bullet.
But understanding cellular signaling may be one of the next frontiers in dermatology.
And exosomes are part of that conversation — cautiously, responsibly, and scientifically.
FAQ
1. Do exosomes really work for melasma and dark spots?
Exosomes show promising early results in reducing inflammation-driven pigmentation, including melasma and stubborn dark spots. Small clinical studies suggest improvement in melanin regulation and skin repair. However, exosome therapy is not a bleaching treatment and should be considered an adjunct to proven therapies such as sunscreen, topical actives, and pigment-control protocols. Larger randomized clinical trials are still needed to confirm long-term effectiveness.
2. Are exosomes safe for darker skin types?
Exosomes may be suitable for darker skin types when used appropriately and sourced from reputable manufacturers. Because melanin-rich skin is more prone to post-inflammatory hyperpigmentation (PIH), the anti-inflammatory signaling properties of exosomes are theoretically beneficial. However, safety depends heavily on delivery method, product quality, and clinical supervision. Injectable human-derived exosome products require careful regulatory consideration.
3. How long does it take to see results from exosome therapy for pigmentation?
Results from exosome therapy are gradual. Most patients notice improvement in skin texture and glow first, followed by subtle softening of pigmentation over several weeks to months. Exosomes regulate cellular signaling rather than directly bleaching pigment, so realistic expectations are essential. Multiple sessions may be required depending on severity.
4. Are exosomes better than PRP for hyperpigmentation?
Exosomes and PRP (platelet-rich plasma) work differently. PRP delivers growth factors from the patient’s own blood, while exosomes deliver signaling molecules that influence cellular communication. Current evidence does not clearly show that exosomes are superior to PRP for pigmentation. They are considered alternative regenerative approaches, and the choice depends on clinical goals, skin type, and practitioner experience.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810