Skin Barrier Damage: Symptoms, Causes, and How to Repair It Scientifically
Table of Contents
Introduction: Why Skin Barrier Damage Is at the Root of Most Skin Problems
Many people believe their skin concerns are separate issues.
Pigmentation. Acne. Sensitivity. Dryness. Burning. Sudden breakouts.
In reality, these problems often share one common root cause: skin barrier damage.
When the skin barrier is compromised, treatments stop working the way they should. Pigmentation becomes harder to fade. Actives sting. Acne worsens instead of improving. Even the best skincare routine starts to fail.
Learn more on why pigmentation treatments fails?
Understanding how the skin barrier works—and how to repair it properly—is essential for long-term skin health, especially if you struggle with pigmentation, melasma, or treatment resistance.
What Is the Skin Barrier?
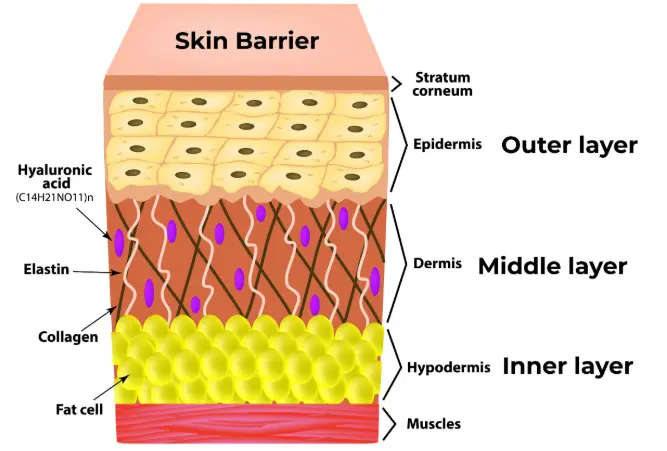
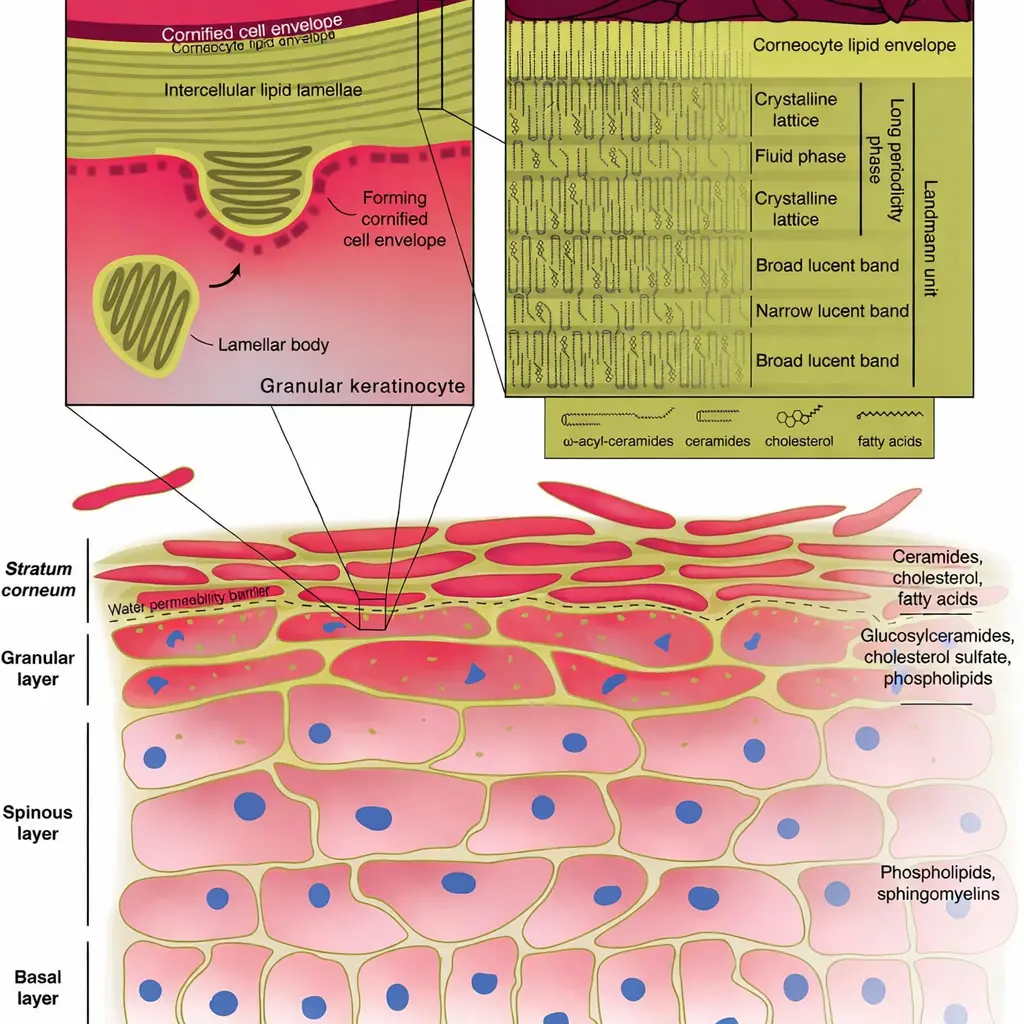
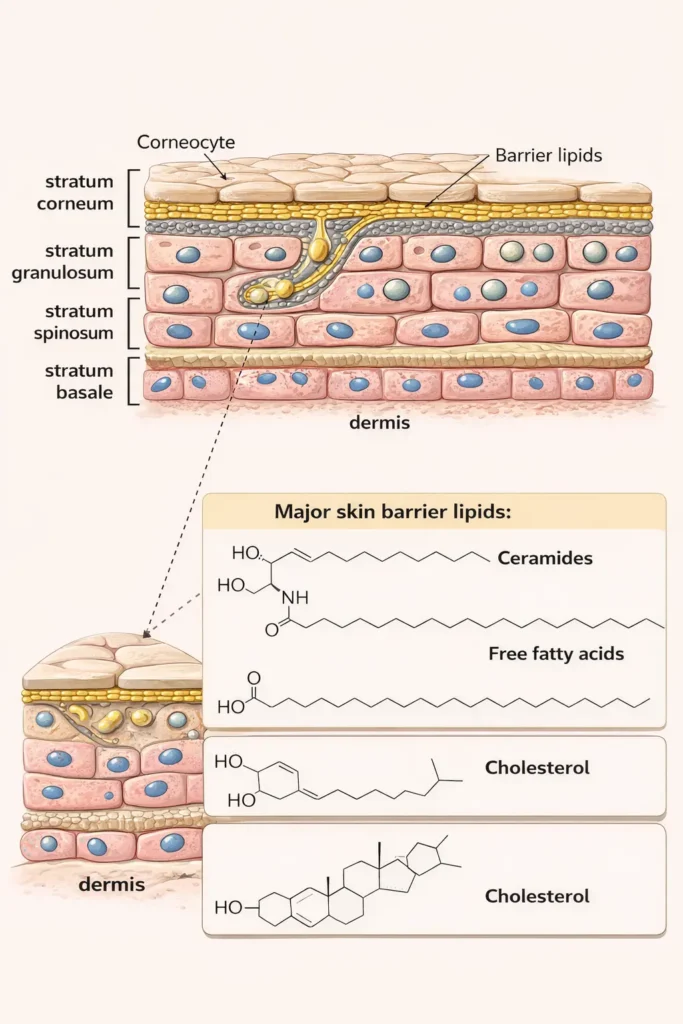
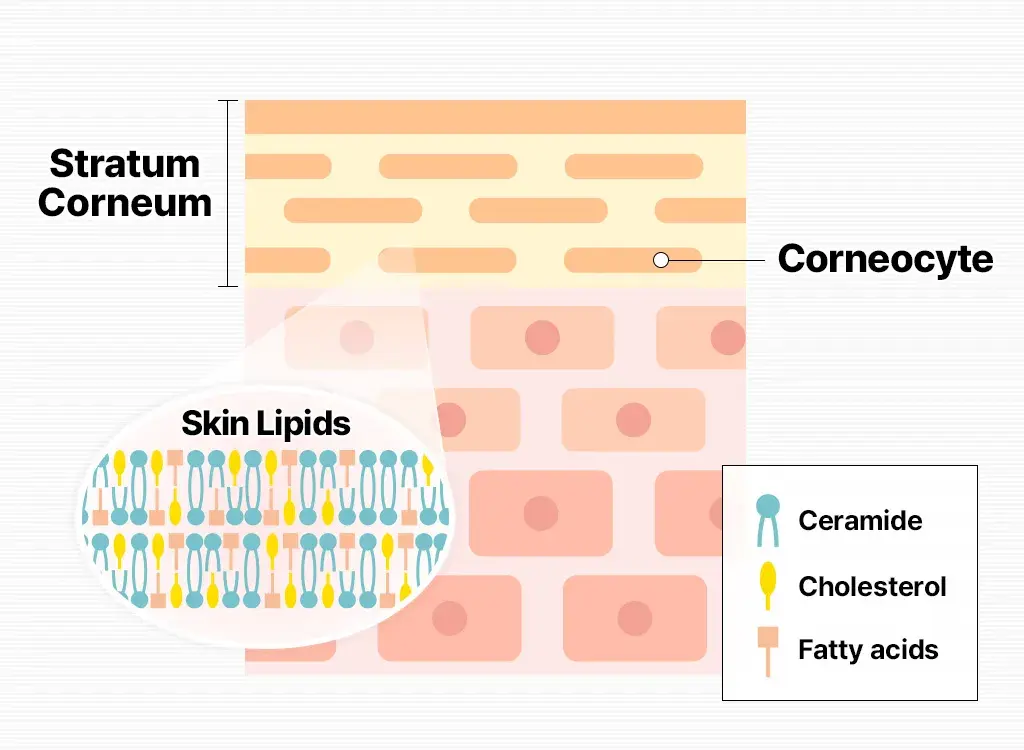
The skin barrier refers primarily to the stratum corneum, the outermost layer of the skin.
It is often described using the brick-and-mortar model:
- Skin cells (corneocytes) act as bricks
- Lipids—ceramides, cholesterol, and fatty acids—act as mortar
Together, they form a protective wall that:
- Prevents water loss
- Blocks irritants and allergens
- Regulates inflammation
- Maintains a stable environment for skin repair
When this structure is intact, skin appears calm, resilient, and responsive to treatment.
Learn more from post-inflammatory hyperpigmentation guide.
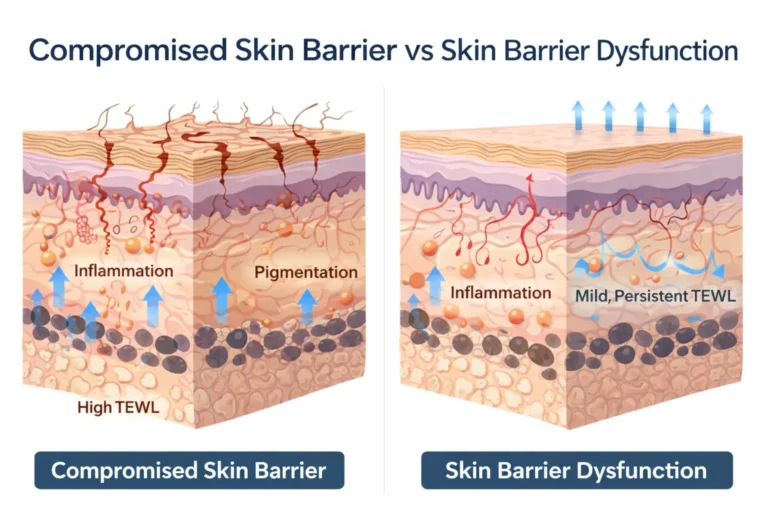
What Happens When the Skin Barrier Is Damaged?
When the lipid structure is disrupted, the skin becomes permeable in the wrong way.
Why pigmentation looks darker before it improves?
This leads to:
- Increased transepidermal water loss (TEWL)
- Easier penetration of irritants
- Chronic low-grade inflammation
- Overactive melanocytes
- Poor tolerance to skincare products
Learn about melanocyte memory and function with pigmentation recurring.
According to dermatologist Dr. Faiza Shams:
“Barrier disruption creates a state of invisible inflammation. Even when the skin looks normal, it behaves reactively, which is why pigmentation and sensitivity often worsen despite treatment.”
Common Symptoms of Skin Barrier Damage

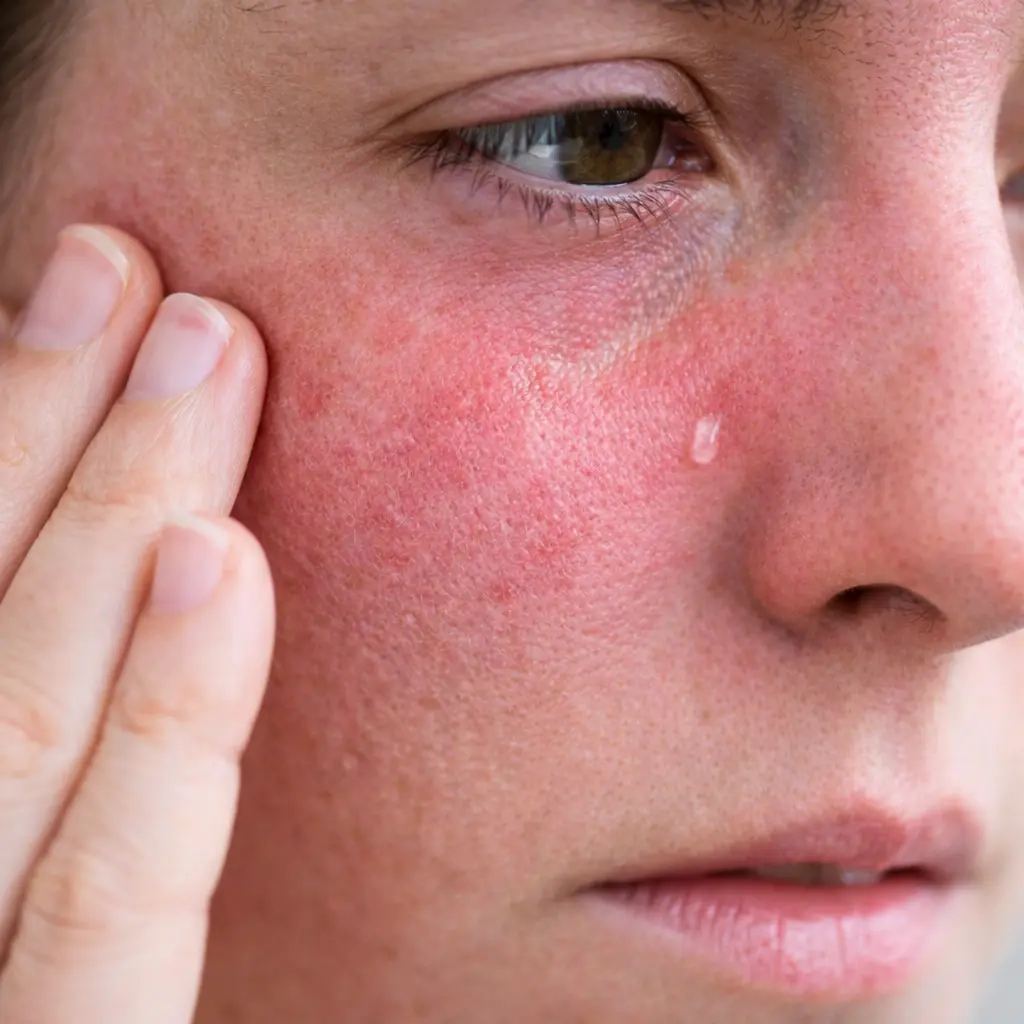
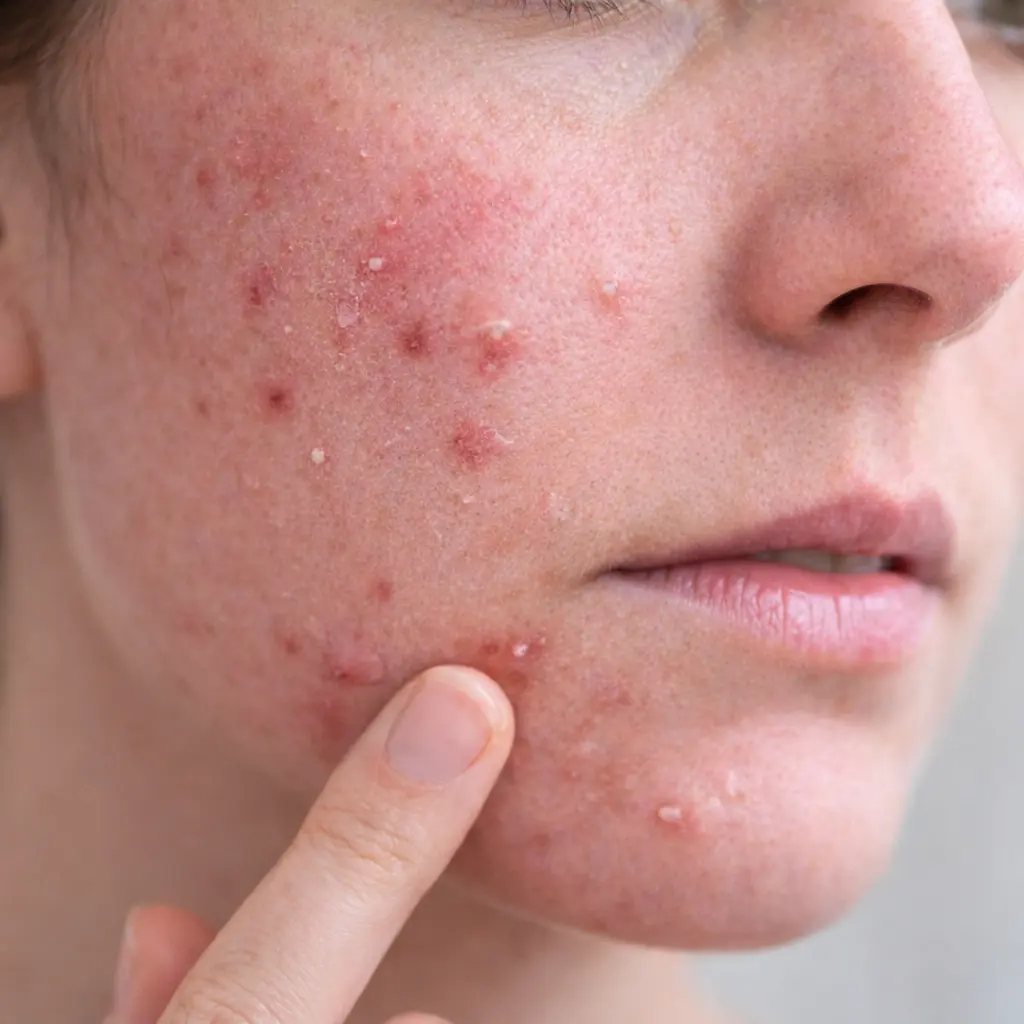
Skin barrier damage does not always look dramatic. In many cases, it is subtle but persistent.
Typical signs include:
- Tightness even after moisturizing
- Burning or stinging with products that previously worked
- Sudden sensitivity to sunlight or heat
- Flaky yet oily skin
- Redness without visible rash
- Acne that worsens with treatment
- Pigmentation that darkens or spreads
These symptoms often coexist, especially in people treating melasma or hyperpigmentation.
Main Causes of Skin Barrier Damage
Over-Exfoliation and Active Overuse
Frequent use of acids, retinoids, scrubs, or peels can strip barrier lipids faster than the skin can replenish them.
Harsh Cleansers
High-foam or sulfate-based cleansers dissolve protective lipids, leaving skin vulnerable.
UV, Heat, and Visible Light
Sun exposure and heat weaken lipid organization and increase inflammatory signaling.
Learn more about visible light and pigmentation.
Environmental Stressors
Pollution, dry climates, and indoor heating disrupt barrier homeostasis.
Inappropriate Skincare Routines
Layering too many actives or following trends without skin-type consideration often leads to barrier collapse.
Learn more about hormonal pigmentation.
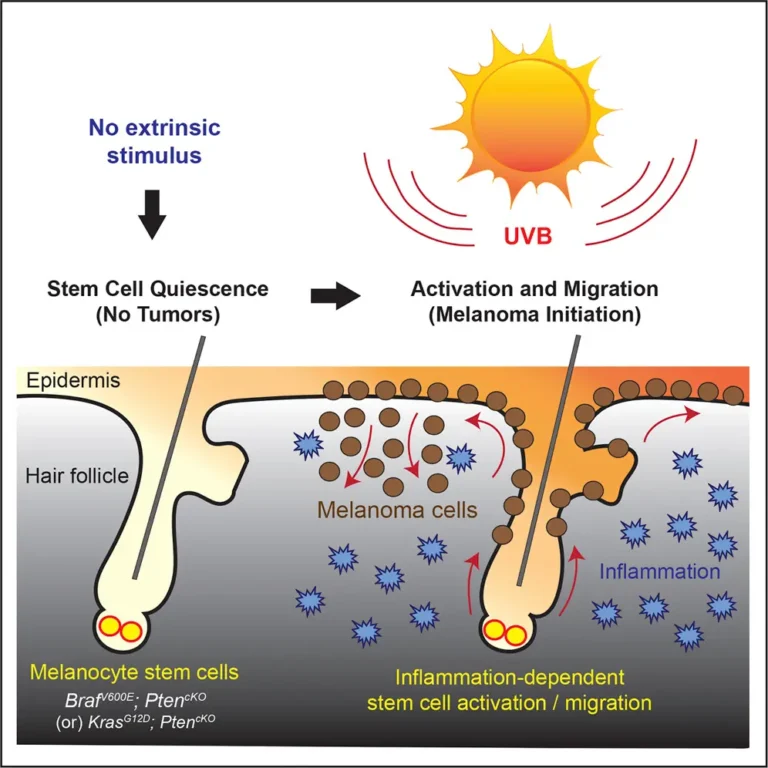
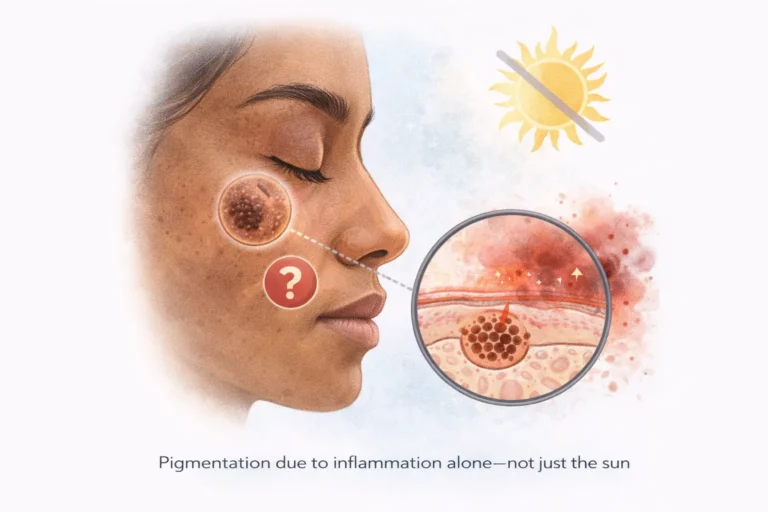
The Link Between Skin Barrier Damage and Pigmentation

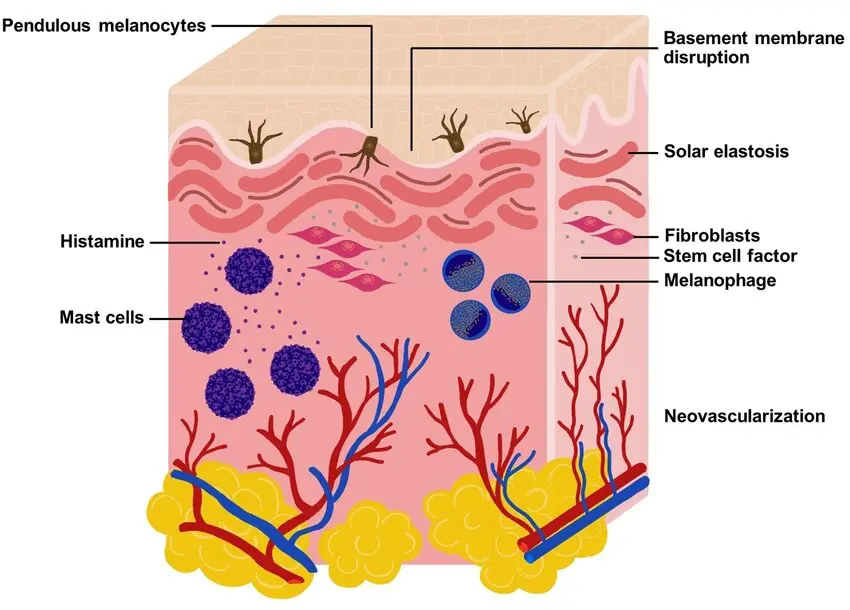
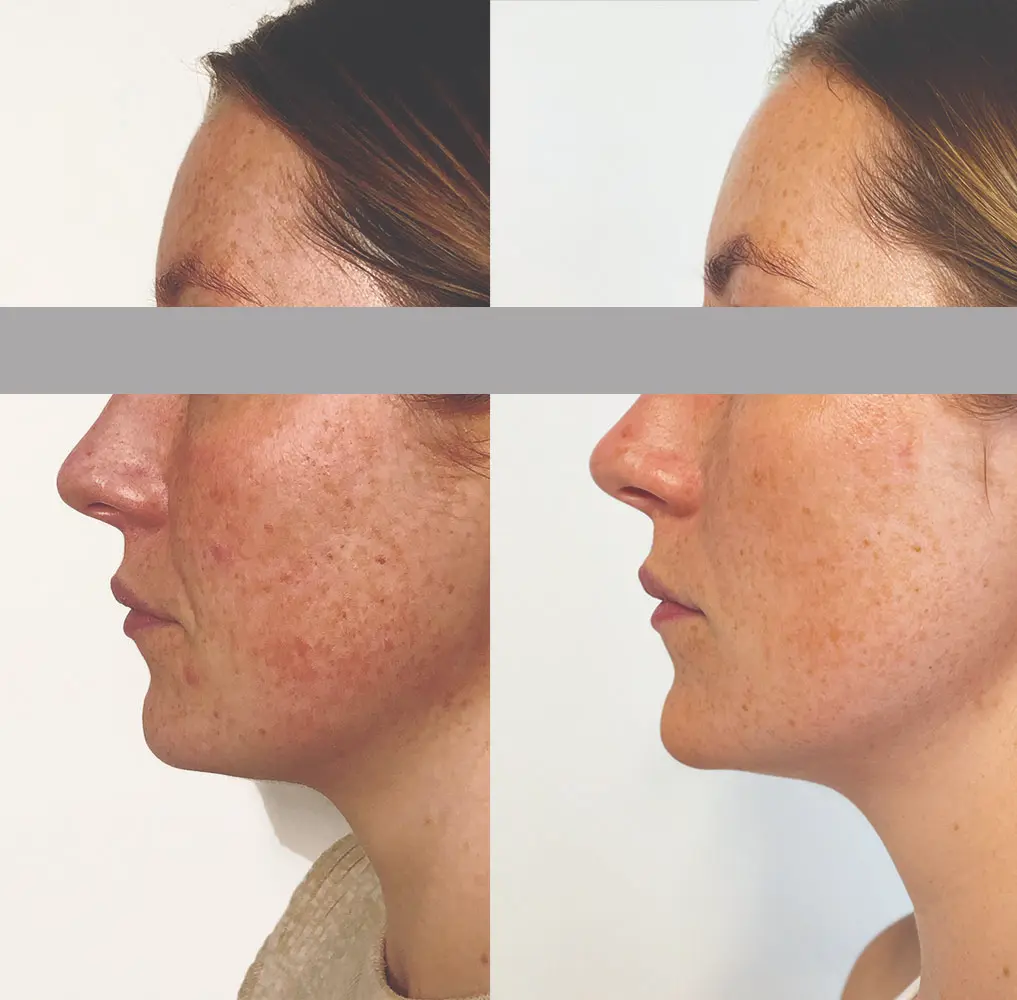
Barrier damage plays a critical role in melasma and post-inflammatory hyperpigmentation.
When the barrier is impaired:
- Inflammation increases
- Melanocytes receive stronger stimulation
- Pigment spreads more easily into surrounding skin
Dr. Faiza Shams explains:
“In melasma-prone skin, barrier damage amplifies pigment signaling. Treating pigmentation without repairing the barrier often leads to relapse or treatment failure.”
This is why pigmentation sometimes appears darker before improving—or fails to improve altogether.
How to Repair the Skin Barrier Scientifically
Repairing the skin barrier is not about using more products.
It is about restoring structure, reducing inflammation, and allowing the skin to normalize.
Step 1: Stop What Is Actively Damaging the Barrier
This may include:
- Daily exfoliation
- Multiple strong actives used together
- Physical scrubs
- Over-cleansing
Temporary reduction does not mean abandoning treatment—it means creating conditions where treatment can work.
Step 2: Use Barrier-Identical Lipids

The skin barrier repairs best when supplied with lipids it recognizes.
These include:
- Ceramides
- Cholesterol
- Free fatty acids
Products containing these in balanced ratios help restore the mortar between skin cells rather than sitting superficially.
Step 3: Reduce Inflammation, Not Just Dryness
Soothing ingredients are critical during repair:
- Panthenol
- Niacinamide (low to moderate concentrations)
- Allantoin
- Colloidal oatmeal
Hydration alone is not enough if inflammation persists.
Step 4: Protect the Barrier From Further Damage
Daily sun protection is non-negotiable.
UV exposure delays barrier repair and worsens pigmentation signaling.
Heat management, gentle cleansing, and avoiding irritants are equally important during recovery.
Complete guide on iron oxide sunscreens.
How Long Does Skin Barrier Repair Take?
Barrier recovery is not instant.
- Mild damage: 1–2 weeks
- Moderate damage: 4–6 weeks
- Chronic damage: 8–12 weeks or longer
Consistency matters more than product quantity.
Can You Repair the Skin Barrier Without Stopping Actives?
In some cases, yes—but only with careful adjustment.
For pigmentation-prone skin:
- Reduce frequency, not necessarily eliminate actives
- Use actives on alternate nights
- Strengthen barrier support on off days
This prevents rebound pigmentation while allowing healing.
Common Myths About Skin Barrier Repair
“Oily skin doesn’t need barrier repair”
False. Oily skin can have a severely damaged barrier masked by excess sebum.
“If it tingles, it’s working”
Persistent stinging is a sign of inflammation, not efficacy.
“More products repair faster”
Layering without strategy often worsens barrier stress.
Why Skin Barrier Repair Improves Every Skin Condition
Once the barrier recovers:
- Pigmentation responds better to treatment
- Acne becomes more manageable
- Sensitivity decreases
- Skin texture improves
- Relapse rates drop
Barrier health determines how well skin heals—and how well treatments perform.
Final Thoughts: Barrier First, Results Follow
Skin barrier damage is not a minor issue.
It is a foundational problem that affects pigmentation, acne, sensitivity, and treatment outcomes.
Repairing the barrier is not a step backward—it is often the missing step.
As Dr. Faiza Shams emphasizes:
“Healthy skin does not come from aggressive treatment. It comes from restoring balance, protecting the barrier, and then treating concerns strategically.”
When the barrier is respected, the skin becomes resilient—and results finally last.
FAQS
1. How do I know if my skin barrier is damaged?
Common signs of a damaged skin barrier include persistent dryness, burning or stinging with skincare products, redness, flaking, increased sensitivity, acne flare-ups, and pigmentation that worsens despite treatment.
2. Can a damaged skin barrier cause hyperpigmentation or melasma?
Yes. Skin barrier damage increases inflammation and melanocyte stimulation, which can worsen melasma and post-inflammatory hyperpigmentation and make pigmentation harder to treat.
3. How long does it take to repair a damaged skin barrier?
Mild barrier damage may improve within 1–2 weeks, while moderate to severe or chronic damage can take 4–12 weeks with consistent barrier-repair skincare and sun protection.
4. Should I stop all active ingredients if my skin barrier is damaged?
Not always. In many cases, reducing frequency and strength of actives while increasing barrier-repair support is more effective than stopping everything completely, especially for pigmentation-prone skin.
5. What ingredients help repair the skin barrier the fastest?
Ceramides, cholesterol, fatty acids, panthenol, niacinamide (low concentrations), glycerin, and soothing agents like colloidal oatmeal are among the most effective ingredients for restoring a damaged skin barrier.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810