Hormonal Pigmentation: How Estrogen, Progesterone, and Cortisol Affect Skin Color
Table of Contents
Many people notice that their pigmentation changes during specific phases of life.
Dark patches appear during pregnancy.
Melasma worsens after starting or stopping birth control.
Pigmentation flares during periods of intense stress.
These patterns are not random.
They are driven by hormonal pigmentation—a form of discoloration that originates from internal biochemical signals rather than surface skin damage.
As Dr. Faiza Shams explains:
“Hormonal pigmentation behaves very differently from sun or acne-related pigmentation. It’s not just about what you apply to the skin—it’s about how internal signals influence melanocyte activity.”
How skin pigmentation forms is a question many readers ask when trying to understand why skin tone changes, dark spots appear, or pigmentation becomes uneven over time. This article explores how hormones affect skin color at a cellular level, why hormonal pigmentation is persistent, and how to manage it realistically using science-backed strategies.
What Is Hormonal Pigmentation?
Hormonal pigmentation refers to skin darkening caused or worsened by fluctuations in hormones such as:
- Estrogen
- Progesterone
- Cortisol
These hormones influence melanocyte activity, vascular signaling, and inflammation—key drivers of melanin production.
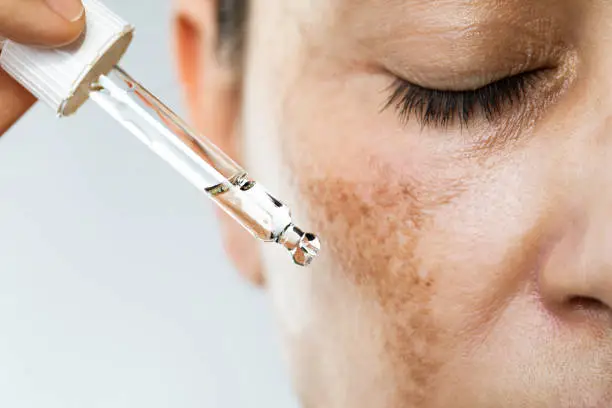
Hormonal pigmentation is most commonly seen as:
- Melasma
- Diffuse facial darkening
- Upper lip and cheek pigmentation
- Pigmentation that worsens cyclically or during stress
Unlike post-inflammatory hyperpigmentation (PIH), hormonal pigmentation often returns even after treatment if the hormonal trigger persists.
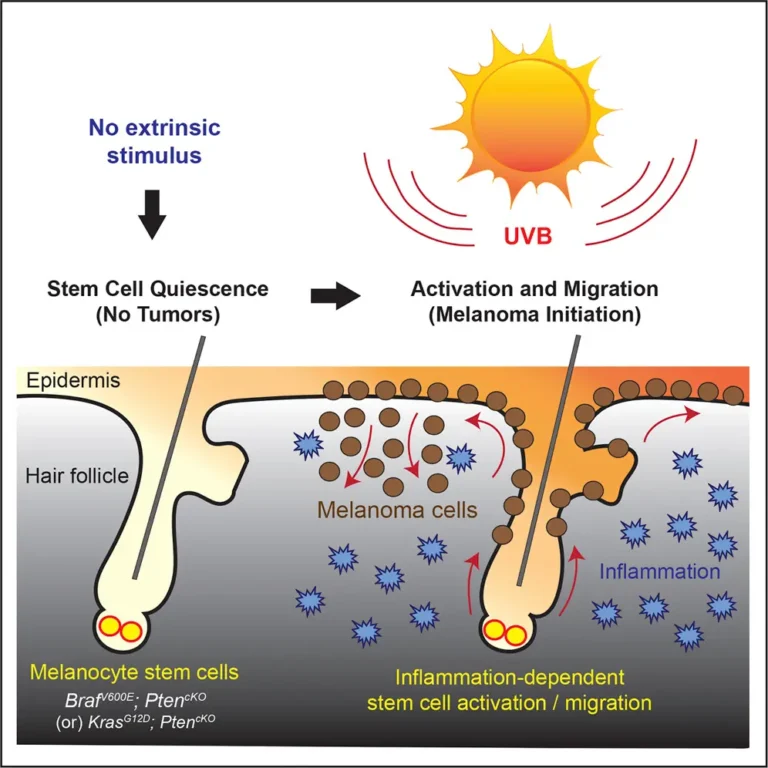
Why Hormones Affect Melanin Production
Melanocytes are not isolated pigment cells.
They respond to hormonal receptors, inflammatory mediators, and vascular signals.
Hormones influence pigmentation by:
- Increasing melanocyte sensitivity
- Enhancing tyrosinase activity
- Prolonging pigment retention
- Amplifying responses to heat and light
This explains why hormonal pigmentation often overlaps with melasma and worsens under environmental stress.
Estrogen and Skin Pigmentation
Estrogen plays the most direct role in hormonal pigmentation.
How Estrogen Triggers Pigment Production
Estrogen:
- Upregulates melanocyte-stimulating pathways
- Increases tyrosinase activity
- Enhances melanin transfer to keratinocytes
Research shows that estrogen receptors are overexpressed in melasma-affected skin, making these areas more reactive.
This is why pigmentation commonly appears or worsens during:
- Pregnancy
- Oral contraceptive use
- Hormone replacement therapy
“Estrogen doesn’t just increase pigment—it increases the skin’s sensitivity to other triggers like heat and visible light,” notes Dr. Faiza Shams.
Progesterone and Pigmentation Persistence
Progesterone does not initiate pigmentation as strongly as estrogen, but it plays a major role in pigment persistence.
Why Progesterone Makes Pigmentation Harder to Fade
Progesterone:
- Stabilizes melanocyte activity
- Reduces natural pigment turnover
- Contributes to vascular changes seen in melasma
This is why pigmentation often:
- Lingers after pregnancy
- Worsens with progesterone-containing contraceptives
- Becomes resistant to topical treatments
Hormonal pigmentation driven by progesterone tends to respond slowly and relapse easily.
Cortisol, Stress, and Pigmentation
Cortisol is the body’s primary stress hormone.
Chronic stress increases cortisol levels, which:
- Weakens the skin barrier
- Increases inflammation
- Enhances melanocyte responsiveness
This creates the perfect environment for pigmentation flares.
“In patients with persistent pigmentation, unmanaged stress is often an overlooked factor. Cortisol-driven inflammation keeps melanocytes activated,” explains Dr. Faiza Shams.
This explains why pigmentation worsens during:
- Emotional stress
- Sleep deprivation
- Illness
- Overtraining
Hormonal Pigmentation vs Other Types of Pigmentation
Hormonal pigmentation behaves differently from other forms.
| Feature | Hormonal Pigmentation | PIH | Sun-Induced Pigmentation |
|---|---|---|---|
| Trigger | Hormonal changes | Inflammation | UV exposure |
| Pattern | Symmetrical patches | Spot-specific | Diffuse or spotty |
| Recurrence | High | Low–moderate | Moderate |
| Response to topicals | Slow | Faster | Moderate |
| Long-term control needed | Yes | Sometimes | Sometimes |
Understanding this difference prevents unrealistic expectations.
Why Hormonal Pigmentation Keeps Coming Back
Why melasma keeps coming back is a common question among readers who notice recurring facial pigmentation despite treatment or periods of improvement. Hormonal pigmentation is chronic, not episodic.
Key reasons for recurrence include:
- Ongoing hormonal fluctuations
- Heightened melanocyte sensitivity
- Vascular and inflammatory involvement
- Interaction with heat and visible light
This is why pigmentation may improve temporarily but return after stopping treatment.
Why Topical Treatments Alone Often Fail
Topical agents can reduce pigment—but they don’t alter hormonal signaling.
Without addressing:
- Heat exposure
- Inflammation
- Barrier health
- Stress levels
pigmentation often relapses.
“Topicals are important, but hormonal pigmentation requires a long-term management mindset rather than a quick-fix approach,” says Dr. Faiza Shams.
Managing Hormonal Pigmentation Effectively
The goal is control, not permanent eradication.
1. Reduce Pigment Reactivity
Use ingredients that calm melanocyte activity:
- Azelaic acid
- Tranexamic acid
- Niacinamide
- Cysteamine
These regulate melanin production rather than aggressively removing pigment.
2. Strengthen the Skin Barrier
A healthy barrier reduces hormonal pigment flares.
Focus on:
- Ceramides
- Panthenol
- Glycerin
Barrier damage amplifies hormonal signaling in the skin.
3. Control Heat and Light Exposure
Hormonal pigmentation is highly sensitive to:
- Heat
- Visible light
Tinted sunscreens with iron oxides are essential.
4. Manage Stress and Lifestyle Factors
While skincare can’t control hormones directly, lifestyle adjustments help:
- Sleep regulation
- Stress reduction
- Avoiding over-exfoliation
These steps lower cortisol-driven pigmentation triggers.
5. Professional Support When Needed
In resistant cases, dermatologists may consider:
- Oral tranexamic acid (under supervision)
- Combination topical therapy
- Long-term maintenance plans
Hormonal pigmentation requires consistency and patience.
Does Hormonal Pigmentation Ever Go Away?
Hormonal pigmentation can:
- Fade significantly
- Become barely visible
- Remain stable for long periods
But it rarely disappears permanently if hormonal triggers persist.
The realistic goal is long-term control with minimal relapse.
Science-Backed Insights You Should Know
Recent dermatology research confirms:
- Estrogen receptors are upregulated in melasma skin
- Progesterone contributes to pigment persistence
- Cortisol amplifies inflammatory pigmentation pathways
- Hormonal pigmentation is vascular and inflammatory, not purely melanin-based
Hormonal pigmentation in Indian skin is a common concern, as higher melanin levels combined with hormonal fluctuations can make pigmentation more noticeable and persistent. These findings explain why hormonal pigmentation behaves differently from other dark spots.
Final Thoughts
Hormonal pigmentation is not a surface problem—it is a systemic skin response influenced by estrogen, progesterone, cortisol, and environmental triggers.
Understanding this shifts expectations and improves outcomes.
As Dr. Faiza Shams summarizes:
“Once patients understand the hormonal nature of their pigmentation, they stop chasing quick fixes and start seeing real, sustainable improvement.”
References
- Passeron T. et al., “Hormonal and Vascular Factors in Melasma,” Journal of the European Academy of Dermatology, 2022–2024.
- Rodrigues M. et al., “Estrogen Receptors and Melanogenesis,” Dermatologic Clinics, 2021–2023.
- Grimes P.E., “Stress, Cortisol, and Pigmentation Disorders,” Journal of Clinical and Aesthetic Dermatology, 2022–2024.
FAQS
1. What is hormonal pigmentation and how is it different from regular hyperpigmentation?
Hormonal pigmentation is caused by internal hormonal fluctuations such as estrogen, progesterone, and cortisol, rather than external triggers like acne or sun exposure. It often appears as symmetrical patches (like melasma) and tends to recur if hormonal triggers persist.
2. Can hormonal imbalance cause pigmentation on the face?
Yes. Hormonal imbalance can directly trigger facial pigmentation by increasing melanocyte activity. Changes during pregnancy, birth control use, menopause, or chronic stress commonly lead to pigmentation due to hormonal imbalance.
3. Why does melasma worsen with hormonal changes?
Melasma worsens with hormonal changes because estrogen and progesterone increase melanocyte sensitivity and pigment production. These hormones also make the skin more reactive to heat and visible light, which further intensifies pigmentation.
4. Does stress and high cortisol levels affect skin pigmentation?
Yes. Chronic stress raises cortisol levels, which weakens the skin barrier and increases inflammation. This environment keeps melanocytes activated, making pigmentation darker and more persistent, especially in hormonally sensitive skin.
5. Can hormonal pigmentation be treated permanently?
Hormonal pigmentation usually cannot be cured permanently if hormonal triggers continue. However, it can be effectively managed long-term with pigment-regulating ingredients, sun and heat protection, stress management, and consistent maintenance routines.
Address: Block C, Punjab University Employees Housing Scheme Phase-II, Lahore, Pakistan
Contact Number: +923224563810